|
Completely oblivious of the implications of her body’s positioning, Rebecca Branagan, 30, reportedly began a lifetime of chronic knee pain by sitting awkwardly for two minutes Tuesday. According to sources, Branagan’s slight five millimeter shift of bodyweight while her knee was folded oddly underneath her for a little over a minute caused irreparable damage to the ligaments that would plague her for the next four or five decades. Several reports confirmed that the suffering triggered by the brief unnatural positioning that would force her to try multiple pain medications to alleviate the agonizing spasms she would get from the moment she woke up until she went to sleep at night would never go away and more likely only worsen until the day she died. At press time, Branagan had stood up from the weird position and started stretching and shaking out her legs to get the strange feeling in her knee to go away. https://www.theonion.com/knee-to-hurt-for-rest-of-life-after-30-year-old-woman-s-1847055269 While The Onion is usually satire, the article is not far from the truth. While the injury of a strained ligament or torn cartilage may not be curable - to the extent that it never happened. Medication may provide some relief but will not cure the problem. Surgery may eventualy be necessary but it will not restore the tissue to new and can often muck things up worse. The goal of therapy would be to stabiize the injury and then maintain it.
Simple guidelines for healthy meals Please note that I am relaying the article. It is not my original composition, yet does articulate dietary goals consistent with my other submissions. The flurry of nutritional information in the media can make healthy meal planning seem daunting and confusing. But it doesn’t have to be, according to Walter Willett, professor of epidemiology and nutrition at Harvard T.H. Chan School of Public Health. He offered a few simple tips in a February 12, 2019 Boston Globe article.
Read the Boston Globe article: What does a healthy meal look like these days? Dr. Wayne Coghlan: ChiropractorManaging the MunchiesCould it be? Something that can help manage the muchies? One of the most weight gaining challenges for myself and common for many people I've talked to is the late night munchies. This is the insatiable craving we get in the evening. We know we've had a good meal. We aren't really hungry and we know we don't need the extra calories. But something in the fridge beacons us like the siren's call. And we open the fridge... then close it. Then open again as if we expect something is magically different. It's calling you. Repeat. Repeat. And it doesn't stop until.. we've eaten the left over roast from Sunday, or the pasta salad from yesterday... emptied the gravy bowl... or sampled the ketchup bottle... or.... And once again another 600 calories has gone down the hatch. The shame of it all. As well as the knowledge that we'd have to walk around Lake Simcoe to burn off that many unnecessary calories. What is going on is the unwanted influence of the the endoocannabinoid system (ECS). The ECS is involved in a variety of physiological processes including appetite, pain-sensation, mood, and memory. The ECS is also involved in voluntary exercise and may be related to the evolution of the runner's high in human beings and related aspects of motivation or reward for locomotor activity in other animals. The ECS is also the part of the nervous system activated by marijuana. Hence the common experience with marijuana users getting the munchies. It seems to be the same craving whether induced by toking... or not. Now the entrepreneurial minded reader would be thinking, "Man, they could make a fortune if they found some drug or something that would block the munchies and effectively suppress appetite. People who struggle with weight would pay $$$ for it, let along the benefits to societal health in terms of the reduce morbidity of excessive body weight." And you would be correct! Click here for the article on weight management and diets. And there has been much research by the big pharmaceutical companies to find a drug to effectively block the ECS. The problem then emerges, that along with blocking appetite, the drugs caused a host of very unpleasant side effects. See the article about Rimonabant. At this time, there is no such drug close to becoming marketable. And as with non-pharmaceutical natural remedies .. .there isn't a lot of help. I expect there are many suggestions from herbal teas to .... ? This article "How to Stop the Munchies When You’re High" basically says if you toke, you're going to get the muchies, without suggesting other remedies. I will pass on three remedies that may help manage the munchies whether from marijuana use... or not. One very sincere lady told me that as soon as she brushes her teeth, the cravings go away. Could it be that simple? An unwanted side effect of marijuana use is Cannabinoid hyperemesis syndrome, characterized by recurrent nausea, vomiting and crampy abdominal pain. These symptoms have been reported to be improved temporarily by taking a hot shower or bath. Perhaps an early evening hot batch can help alleviate non-marijuana induced munchies. And now... Walnuts ... keep reading..... Dr. Wayne Coghlan: ChiropractorWalnuts may reduce the Munchies!!
DIET OBESITY METABOLISM WALNUTS METABOLIC DISEASE WEIGHT LOSS DIABETES FOOD
Original source by MARIELLE MONDON, PhillyVoice Staff. AUGUST 20, 2017 For people looking to cut back on food cravings, a daily handful of walnuts could have significant and lasting effects. A recent study published in the journal Diabetes, Obesity and Metabolism looked at the walnut effect on hospitalized obese subjects who were treated with a smoothie containing 48 grams of walnuts. Of the 10 patients, half were instead given a placebo smoothie with no walnut content. A month later the placebo patients were served the walnut shake and vice versa. Later, researchers ran MRI exams while showing patients photos of both healthy food and high-fat food, as well as neutral pictures. The MRI exams showed that those treated with the walnut smoothie had better impulse control than those treated with the placebo. Insula, the part of the brain related to impulse control, increased among drinkers of the walnut smoothie but not among the placebo drinkers. “Walnuts can alter the way our brains view food and impact our appetites,” said lead author Olivia M. Farr to the New York Times. Farr works at Beth Israel Deaconess Medical Center in Boston. “Our results confirm the current recommendations to include walnuts as part of a healthy diet.” In addition to being a good diet food control hack, walnuts are also linked to treating type 2 diabetes. The study was supported by a Harvard Clinical and Translational Science Center Grant and an NIH grant. The California Walnut Commission also supported -- but did not design or conduct -- the study. Here is a link to the originating article. Walnut consumption increases activation of the insula to highly desirable food cues: A randomized, double-blind, placebo-controlled, cross-over fMRI study. First published: 17 August 2017 DOI: 10.1111/dom.13060 Dr. Wayne Coghlan: ChiropractorFree Consultationdrwaynecoghlan.weebly.com
YOU'RE NOT SURE THAT CHIROPRACTIC CAN HELP YOU!
CAN YOU HAVE A NO COST CONSULTATION?
Connection: Dr. Wayne Coghlan [email protected] (c) 705 446 7003
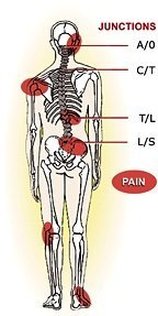
NP = Notalgia (Greek for pain in the back) Paresthetica (a sensation of pricking, tingling, or creeping on the skin that has no objective cause) is nothing new. The condition was first identified in medical literature by a neurologist from St. Petersburg, Russia in 1934. It has, nevertheless, likely been around since humans started walking upright and may be the reason back scratchers .... or long finger nails were invented. One wonders if bears scratching up against a tree are afflicted with the same curse. NP is characterized by pain, numbness, and itching between the inside edge of the scapula (shoulder blade) and the spine. It is typically on the left side - less often on the right side - and some 10% of presentations are on both sides. It is fairly common condition with a low grade irritation that comes and goes, and most will not bother to report the nuisance to their physician. In fact, many physicians are unfamiliar with NP as a clinical problem. However, for some people the irritation becomes distracting to the point of interference with life quality. As with any irritation, a scratch may give temporary distraction, but scratching creates a secondary inflammation response in the skin... which then makes the itching worse! (This is the same reason that a mosquito bite does get itchier each time you scratch it). So it gets to be a progressive cycle of itching - scratching - more itching - more scratching. With persistent scratching and rubbing over a longer period of time, the skin begins to change, becoming thicker, rougher, and discoloured ... resembling a patch of psoriasis. The irritated skin then becomes its own source of annoyance regardless of the NP being underlying cause. Scratching the skin can also create access for bacteria and lead to secondary infections. For some people the irritation becomes a psychological fixation which further amplifies the awareness of the discomfort due to the effects of the underlying NP. NP itself is not a dangerous condition. It is the nuisance to the point of distraction, repeated scratching, development of secondary effects of skin irritation and perhaps infection, and perhaps depression that become problematic. There is no definitive cause for the condition. Speculation ranges from an overly dense concentration of itch sensitive nerve fibers in the area, to degenerative changes at a cellular level of the skin. It is quite possible that those changes are brought on by the rubbing to relieve the condition, rather than being the cause of NP. Treatments are typically directed at relieving the secondary symptoms of skin irritation and numbing the primary itching. Counter irritants such as capsicum ointment may give the brain something to attend to rather than the more annoying itch. Extreme cases have resorted to more extreme methods of relief such as surgical destruction of the affected nerves. Various medications acting on nerve pain and antidepressants such as amitriptyline may help. While these methods may be well intentioned and variably helpful, they are at best, it seems, only chasing the problem. Please note: Numbness, itching, irritation, and pain can be symptoms of nerve compression and/or irritation. NP is most commonly seen in individuals with some type of neck trouble and potentially a history of whiplash, car accident(s), heavy lifting, computer work, other neck injuries, arthritis, fibromyalgia, and hypertense muscles. There is a positive correlation between the presence and severity of NP with the presence and severity of spinal degenerative arthritis. The theory is that conditions such as poor posture habits, upper body weakness, upper cross syndrome, occupational stress, tech/text neck create cumulative strain and micro trauma. Typically there is increasing inflammation of the muscles of the neck and back, along with advancing degenerative changes in the both the cervical and thoracic spine. When there is stress on the muscles and joints of the spine, fibers of the nerves that provide sensation to the skin of the back can become compressed and/or irritated due to herniated or bulging discs and degenerative arthritis, and/or sustain traction/compression /irritation as they progress through chronically strained and irritated muscles of the upper back. Many people have experienced relief/reduction of NP after spinal manipulative therapy and supportive physical therapy to correct posture, spinal mechanics, and relieve nerve compression. This supports NP as being caused by mechanical stress on the cutaneous branches of the thoracic nerves. There is a similar condition of pain and itching of the arms called Brachioradial pruritus (sometimes abbreviated BRP) that has been successfully treated by spinal manipulative therapy. Spinal manipulative therapy is a method that chiropractors use to "adjust" the alignment of the bones (vertebrae) of the spine. This re-aligns and opens the joints to relieve pressure and irritation of the nerves and other pain sensitive tissues. Certainly correcting spinal alignment and managing ongoing postural and physical stresses is beneficial to any patient…and if it is successful in providing relief of compressed and irritated nerves, it would help the patient manage the cause of NP rather than just chasing it symptomatically. NP tends to be a chronic condition with periodic remissions and flareups. Very early stages of NP may clear fully with appropriate spine therapy, and lifestyle and posture modifications. For more advanced cases with underlying neck and upper back nerve issues, NP it is not necessarily curable but may be controllable. If you, or someone you care about, is suffering from Notalgia Paresthetica, neuralgia, or some other condition related to spinal misalignment and strain. why not explore chiropractic as a possible answer?
Best regards, Dr. Wayne Coghlan. Chiropractor. [email protected] drwaynecoghlan.weebly.com.
It has been my experience that there is a wealth of mis-information regarding many aspects of nutrition. Much of it may be well intended yet ill-informed and mis-guided, yet much is just blatantly wrong and based on wishful thinking, or taking a shred of truth and basing recommendations out of the greater context of intelligent and well researched information. Many so called internet experts don't know what they don't know. It is refreshing then, to come across credible information from people who know what they are talking about.
This article is originally publish as: Susan Roberts, PhD True or False? What Your Older Patients Believe About Nutrition by MedPage Today. at http://www.medpagetoday.com/resource-center/Nutrition-in-the-Elderly/True-or-False/a/58560 As the information is concise I am taking liberty to re-post it here. I there is any conflict, kindly advise.
Should aging adults take multivitamins?
Accessed from: http://www.medpagetoday.com/resource-center/Nutrition-in-the-Elderly/Multivitamins/a/59598?xid=NL_MPT_elderlynutrition_2016-08-22&eun=g622342d0r Edits in italics.
Should Aging Adults Take Multivitamins?
Tracy Hampton, PhD Reviewed by Jackie Ballou Erdos, MS, RD, CSSD, Registered Dietitian & Owner, Balancing Act Nutrition, New York, NYIN BRIEF
Changes associated with normal aging and age-related diseases can impact the nutritional intake of older adults, which in turn affects aspects of health ranging from cardiovascular function to cognition. As the years pass, many may wonder whether they should take a daily multivitamin to fill any gaps in their diet. “For very healthy patientshttp://24636538-181122512915269833.preview.editmysite.com/editor/main.php# with a great diet, a multivitamin may not be necessary; however, a simple multivitamin is unlikely to hurt either, so it becomes a personal choice,” said Katherine Tucker, PhD, a Professor of Nutritional Epidemiology in the Department of Clinical Laboratory & Nutritional Sciences at UMass Lowell. However, as we age, our need for calories decreases while our need for nutrition increases. “As nutrient inadequacies are more common with aging, though, a multivitamin supplement may be useful for many individuals, particularly if the diet is not adequate in nutrient quality or quantity.” Multiple factors come into play when considering the nutritional needs of older and elderly adults—for example, their specific health conditions, activity level, caloric requirements, and ability to access and prepare food (not to mention their personal food preferences) will shift over time and have varying effects on their dietary intake. Tucker noted that aging is often associated with a decreased sense of smell and appetite that may lead to inadequate nutrient intake, as well as malabsorption of nutrients that can decrease the health benefits of consumed foods. “Therefore, at the same time that energy requirement is decreasing, the need for many specific nutrients is increasing,” she said. “Vitamin B12, for example, is a common deficiency due to poor absorption as stomach acid decreases. This means that it is very important to choose nutrient-dense foods and to avoid empty calorie foods and, in cases of deficiency, supplements may be needed.” Numerous observational studies looking at the effects of multivitamins on overall health as well as on specific health parameters have generated conflicting results. “The observational studies evaluating multivitamin use on various health outcomes have been mixed, but there are many methodologic limitations that have not been fully accounted for,” said Howard Sesso, ScD, MPH, an Associate Epidemiologist at the Divisions of Preventive Medicine and Aging at Brigham and Women’s Hospital, and an Associate Professor of Medicine at Harvard Medical School. “For example, there are hundreds of multivitamin formulations on the market, making it difficult generalize multivitamin as a single category. We also know that those taking multivitamins may differ in important ways compared to non-users that observational studies try, but probably don’t optimally, account for,” he says. The best evidence for any effects of a multivitamin on health comes from randomized clinical trials, for which only one long-term, large-scale trial—the Physicians’ Health Study II (PHS II), which included men aged 50 years and older—has been completed. A 2012 analysis of PHS II by Sesso and his colleagues found that multivitamins did not reduce major cardiovascular events, including myocardial infarction, stroke, and cardiovascular mortality, after more than a decade of treatment and follow-up.1 Daily multivitamin supplementation in PHS II has been found to modestly but significantly reduce the risk of total cancer.2 In addition, daily multivitamin use modestly and significantly decreased the risk of cataracts, but had no significant effect on visually significant age-related macular degeneration.3 Among male physicians aged 65 years or older in PHS II, long-term use of a daily multivitamin did not provide cognitive benefits.4 “We recently initiated a new clinical trial, the COcoa Supplement and Multivitamin Outcomes Study, or COSMOS, to examine the long-term health effects of multivitamin use in older women, plus see whether we can replicate in women the encouraging findings on cancer and cataract seen in PHS II,” said Sesso. Although benefits of multivitamins may only be modest at best in healthy individuals, supplements containing combinations of certain nutrients can provide clear benefits for those who have, or are at high risk for, deficiencies.5 “In a patient with poor health status, nutrient status should be checked,” said Tucker. “Nutrient supplements make a big difference if there are deficiencies; however, too many supplements may also be harmful.” Tucker pointed to deficiencies in vitamins B12 and D as common among older patients, noting that these vitamins may need to be taken in doses higher than those contained in a standard multivitamin. On the other hand, care should be taken to avoid too much folic acid, iron, and preformed vitamin A, or retinol. “The major multivitamin brands tend to represent safe products, so there is likely no downside to taking a multivitamin in addition to maintaining a healthy lifestyle and diet,” said Sesso. “But it remains unclear whether taking a multivitamin actually reduces disease risk, though PHS II did provide encouraging data that warrants replication.” As a footnote, many health professionals look to reputable sites like these to ensure that supplement has been tested for purity and to ensure the amount listed on the label matches the amount in the supplement: Consumer Labs NSF Natural Medicine Database Published: 08/09/2016 References:
Dr. Wayne Coghlan: ChiropractorWhen To Use Heat Or Ice To Treat An InjuryWhen to use heat or ice to treat an injury
Applications of hot and cold have been used since antiquity for the treatment of musculoskeletal injuries. The research based evidence and understanding of the complex physiological actions is highly variable *3 as studies will often focus on one aspect of cryo/thermotherapy which may not be applicable to the generalities of the application.. and there is not a lot of money/reward$ in investigating something you can get out of the freezer or the tap.
Clinical wisdom is thus a matter of research as available, intuition, experience, and consensus. Cryotherapy = the application of cold for the treatment of injury or disease. Thermotherapy = the application of heat for the treatment of injury or disease. The benefits of cryotherapy includes:
**** Using a cold compress can also reduce the pain, swelling, and inflammation associated with gout and rheumatoid arthritis. A gentle approach is recommended. ***** Generally speaking, the newer and more severe the injury, and the more pain and swelling associated with the injury, the more you would use ice. The sooner ice can be applied, the better the overall results in terms of stabilizing the injury and promoting recovery. For a new injury remember RICE: Rest, Ice, Compression, and Elevation *1 The importance of rest and accompanying elevation of the limb cannot be ignored *1. Elevation serves to rest the injured area, and utilizes gravity to drain excessive blood from the swollen area. Various methods such as ice packs, ice towels, ice massage, gel packs, refrigerant sprays and inflatable splints can be used each with their own pros/cons.
Topical cold treatment decreases the temperature of the skin and underlying tissues to a depth of 2
to 4 cm. I recommend applying the ice on/off for 10-20 minute intervals. Use shorter intervals for smaller joints and injuries with less insulation of skin fat. For larger and deeper areas use the ice longer. If the skin becomes firm or pressing your finger into the skin leaves a lingering pale spot, give the area a rest or warm with your hand for a few minutes to avoid frost-bite. The tissue below the skin will remain effectively chilled for up to 20 minutes. To my understanding, the use of "ice gels" such as Deep Ice and Deep Cold may be cooling to the skin and soothe the pain of an acute injury, but I have not seen any evidence that they effectively cool an injury below the skin level. At best they are a comfort due to the counter irritation of the skin , but not an effective treatment. For new injuries continue applying ice for the first two to three days. Traditional wisdom recommends that beginning about two days after the injury, one would begin alternating applications of heat then ice... always finishing with ice. Nadler reports that contrast therapy (alternating between hot and cold treatment) provides no additional therapeutic benefits compared with cryotherapy or thermotherapy alone *2. It seems that alternating from heat to ice for short periods just keeps the internal tissue temperature near normal. Perhaps applying heat for 20 minutes, rest 20 minutes, ice 20 minutes, rest 20 minutes ...repeat... may have a net therapeutic effect of drawing fresh blood into the injury and promoting increase metabolism to stimulate healing, then using ice to prevent excessive swelling and inflammation. Opportunity for some research! Nonetheless.... As you continue into the rehabilitation stage of the injury, use elevation and ice after exercise for as long as pain and swelling persist. Cold appears to be effective and harmless and few complications or side-effects after the use of cold therapy are reported. However, prolonged application at very low temperatures should, however, be avoided as this may cause serious side-effects, such as frost-bite and nerve injuries.
Although cold and hot treatment applications both decrease pain and muscle spasm, they have opposite effects on tissue metabolism, blood flow, inflammation, edema, and connective tissue extensibility. Cryotherapy decreases these effects while thermotherapy increases them.
The conventional wisdom is to use heat to soothe an older injury. This largely due to the reduction in muscle spasm due to increased blood flow, and reduced pain sensation largely due to the stimulation of superficial nerves rather than physiologic effects in the deeper tissue. Using heat may stimulate healing and repair of new and old injuries in combination with active exercise and tools such as ultrasound and shock-wave therapy. Heat can be applied in numerous ways from convenient gel packs to hot water bottles to heat baths to electrically insulated heating pads. Using a moist towel between the heat source and your skin can help the heat penetrate the tissue.
*3 Upon reviewing the literature much of the confusion arises from the limiting nature of studying heat and ice on injuries... how does one ethically and practically use sham heat or ice? Another limit is that many studies have very specific research parameters that do not necessarily translate to clinical use. Nevertheless.... apply heat or ice with caution and some good sense. If you are unsure consult with your health professional. Dr. Wayne Coghlan: Chiropractor. drwaynecoghlan.com. Email: [email protected]
REFERENCES:
Scott F. Nadler, DO, FACSM, Kurt Weingand, PhD, DVM, and Roger J. Kruse, MD, Cryotherapy and Thermotherapy for the Pain Practitioner. Pain Physician Vol. 7, No. 3, 2004. 395-399. Swenson, C., Swärd, L. and Karlsson, J. (1996), Cryotherapy in sports medicine. Scandinavian Journal of Medicine & Science in Sports, 6: 193–200. doi: 10.1111/j.1600-0838.1996.tb00090.x
FAQs: Frequently asked questions
WHERE IS MY PRACTICE? Dr. Wayne Coghlan is currently in association with Real Rehab and Wellness 1224 Dundas Street West, Unit 102 Mississauga, ON, L5C 1E2 905-273-0088 EMAIL: [email protected] Directions Top Rehab Wellness 512 Bristol Rd W #11b, Mississauga, ON L5R 3Z1, Canada 1 905-507-1808 EMAIL: [email protected] Directions and PhysioFlex 19 Woodbine Downs Blvd, Etobicoke, ON M9W 6N5 (416) 798-8809 EMAIL: [email protected] Directions DO YOU NEED A MEDICAL REFERRAL?
WHAT ARE MY FEES?
WHAT HAPPENS AT YOUR FIRST VISIT?
DO WE TAKE X-RAYS?
study. Dr. Kassis is usually amenable to ordering x-rays of her current patients.
WHAT’S HAPPENS NEXT?
HOW LONG WILL IT TAKE UNTIL YOU ARE BETTER?
DO CHIROPRACTORS ONLY TREAT INJURIES?
WHAT TYPE OF TREATMENT DO I USE?
HOW DOES MANIPULATION WORK?
IS MANIPULATION SAFE?
DOES IT HURT?
DO YOU NEED TO KEEP COMING BACK?
For patients seeking Spinal Correction Care and Wellness Care the course of therapy may vary from Injury Care. DOES OHIP COVER ANY OF THE COST?
DO WE ACCEPT PRIVATE INSURANCE?
INFORMED CONSENT TO CHIROPRACTIC TREATMENT
It is important for you to consider the benefits, risks and alternatives to the treatment options offered by your chiropractor and to make an informed decision about proceeding with treatment. Chiropractic treatment includes adjustment, manipulation and mobilization of the spine and other joints of the body, soft-tissue techniques such as massage, and other forms of therapy including, but not limited to, electrical or light therapy and exercise. Benefits: Chiropractic treatment has been demonstrated to be effective for complaints of the neck, back and other areas of the body caused by nerves, muscles, joints and related tissues. Treatment by your chiropractor can relieve pain, including headache, altered sensation, muscle stiffness and spasm. It can also increase mobility, improve function, and reduce or eliminate the need for drugs or surgery. Risks: The risks associated with chiropractic treatment vary according to each patient’s condition as well as the location and type of treatment.
- The consequences of disc injury or aggravating a pre-existing disc condition will vary with each patient. In the most severe cases, patient symptoms may include impaired back or neck mobility, radiating pain and numbness into the legs or arms, impaired bowel or bladder function, or impaired leg or arm function. - In rare cases, surgery may be needed.
- Chiropractic treatment has also been associated with stroke. However, that association occurs very infrequently, and may be explained because an artery was already damaged and the patient was progressing toward a stroke when the patient consulted the chiropractor. Present medical and scientific evidence does not establish that chiropractic treatment causes either damage to an artery or stroke. - The consequences of a stroke can be very serious, including significant impairment of vision, speech, balance and brain function, as well as paralysis or death. Alternatives: Alternatives to chiropractic treatment may include consulting other health professionals. Your chiropractor may also prescribe rest without treatment, or exercise with or without treatment. Questions or Concerns: You are encouraged to ask questions at any time regarding your assessment and treatment. Bring any concerns you have to the chiropractor’s attention. If you are not comfortable, you may stop treatment at any time. Please be involved in and responsible for your care.
The Frog in the Kettle: There is an old fable about taking a frog from a cool pond and plopping it into warm water. The change in temperature is so abrupt that it alarms the frog and it will jump out to safety. Now take the same frog, place it in a pot of tepid water, and turn the heat on very low. Because the water warms up so very gradually, the frog is not immediately alarmed and will very comfortably tolerate the danger... and eventually gets cooked.
One more illustration to run by you. It takes very little effort, time, and money to allow a house to deteriorate. You ignore the moisture in the windows, don't get around to repairing the loose shingles, the pipes... well.. they are only a little leaky. Eventually, the house is no longer fit to live in. However, a house you can move out of. Your body has to last as long as you live in it. Yes, it does take some investment of time, effort... and money... to keep your home in good shape.... and fit and comfortable to live in.
Important - learn the difference between a traumatic (sports) injury and deteriorative (old sport) injury.
Traumatic injuries can be bad, but if the person is generally healthy and the tissue is in good shape, sudden overloading of the tissue responds well to therapy and heals well. Deteriorative injuries develop insidiously. Often there can be years of wearing and over strain. The tissue doesn't exactly develop inflammation. Rather, the cell and fiber structure break down and the tissue becomes gristly. Eventually there is not enough healthy tissue to sustain the strain and the tissue gives way. In these cases, the problem of repairing the injury is complicated by having so little healthy tissue to work with. Compare a brand new rubber band with one left in the sun a few days, and you get the picture.
** How do I injure thee... let me count the ways.... Headache, migraine, cervical degenerative arthritis, neck and shoulder tension, stress, rotator cuff injury, medial epicondylitis (golfer's elbow), lateral epicondylitis (tennis elbow), carpel tunnel syndrome, wrist fatigue, chest congestion, thoracic spine injury, low back strain, varicose veins, lymphadema, patelo-femoral pain syndrome, ischial bursitis, piriformis syndrome, digestive upset, depression, temporal-mandibular joint syndrome (TMJ).
Short leg syndrome
"The term syndrome refers to the association of characteristics that often occur together, so that the presence of one feature alerts the physician to the presence of the others." Wikipedia.
 Short leg syndrome Short leg syndrome
Standing upright when one leg is shorter is the equivalent of standing sideways on a hill. The person cannot help but lean to the shorter side. The spine may compensate, to limit leaning to the short side, by tilting the upper body in the opposite direction. This produces a "scoliosis" or sideways deviation of the spine. NOT GOOD.
Often a person will try to compensate for a short leg by perching on short leg, usually with the other (longer) leg bent at the knee and turned out... effectively shortening the long leg. NOT GOOD. Rather than balancing the pelvis, fatigue and strain usually causes the pelvis to over compensate. In either case, the distortion of the spine unevenly loads the joints and muscles, and promotes faster wear and tear, and injury. You may have heard of the If you, or someone you care about, is persistently perching on one leg, or complaining of back pain, this needs to be evaluated. The sooner the better The sooner the better. How to manage short leg syndrome: Perching on one leg, postural deviation, spinal scoliosis are a few of the more obvious ways to bring attention to a potentially short leg. I will also have the patient lie both prone and supine and check the leg lengths. Sometimes a leg only appears short due to a distortion in the body alignment. Correcting posture and balancing out the body will usually relieve and functional short leg. The most accurate way to evaluate leg length is to take an x-ray of the pelvis while you are standing....however... I will rarely order an x-ray for this purpose alone. Usually, I make a clinical decision. The easiest method to then manage the leg length discrepancy is to add a shim... or heel lift to the shoe. A simple and inexpensive cork wedge might do the trick. A heel lift can also be added to custom foot orthotics which may be necessary and beneficial to control the mechanics of the foot and its effects on the ascending kinetic chain (check out the video below) . You can only add up to a 7 mm thick lift inside the shoe before the shoe becomes ill fitting and is prone to slipping. Larger leg length discrepancies require additional material to be added to the outside of the heel, usually by a shoe repair professional. Such external lifts are well tolerated and can only be seen when a person is looking for them.
Once the leg length is corrected, a progressive program of chiropractic spinal care can then help correct distorted body mechanics.... and rejuvenate your physical well being.
Read this article on how neglecting the warning signs of a short leg can lead to a permanent deteriorative injury. CLICK HERE.
Dr. Wayne Coghlan: ChiropractorNutritional Intelligence Really? What science says you should eat... Really? What science says you should eat...
What
Science Says You Should Eat Posted by Dr. Wayne Coghlan on drwaynecoghlan.blogspot.com Reposted from original article By Brad Lemley, Photography by Dan Winters From Discover Magazine, February 2004 issue, http://discovermagazine.com/2004/feb/science-diet/article_view?b_start:int=0&-C= This is an edited version of the original article. If you are keen to understand nutrition and the complexity of the myriad of recommendations, then please put the time into reading the article. If you wish my executive summary, please scan down to the end. Most diets aren't realistic or advisable, including the U.S. agriculture department's famous food pyramid. Instead, a Harvard scientist recommends a new way of eating based on the world's largest and longest food study. America clearly needs dietary guidance. More than 44 million people are clinically obese compared with 30 million a decade ago, putting them at increased risk for heart disease, stroke, type 2 diabetes, and breast, prostate, and colon cancers. In the meantime, the noun diet seems to attract a different adjective every week, including Atkins, Ornish, Cooper, grapefruit, rice, protein, Scarsdale, South Beach, Beverly Hills, Best Chance, Eat Smart, and Miracle, not to mention Help, I’m Southern and I Can’t Stop Eating. While some of these plans overlap, others seem to specifically contradict each other, notably the meat-intensive regime of the late Robert Atkins versus the near-vegetarian program of Dean Ornish. No wonder Americans are tempted to follow Mark Twain’s admonition to “eat what you like and let the food fight it out inside.” But still, we wonder: Is there really an optimum way to eat? Although debate rages, academic nutrition researchers have begun to form a consensus around a plan with an important advantage—it is based on a preponderance of sound science. The regime does not as yet have a name, but it might well be called the Willett diet, after its leading proponent, Walter Willett, chairman of the department of nutrition at the Harvard School of Public Health. Featuring abundant fruits, vegetables, whole grains, and vegetable oils, as well as optional portions of fish and chicken, Willett’s plan resembles the much-touted Mediterranean diet shown in several studies to reduce the risk of heart disease. Nonetheless, Willett resists the comparison. “The Mediterranean diet is specific to a certain climate and culture,” he says, adding that by focusing on healthy ingredients rather than specific dishes, “anyone can adapt this plan to his own tastes.” The results: stable blood-sugar levels, easier weight control, clearer arteries, and overall better health. In this case it’s hard science, not just opinion. Willett’s plan is based on the largest long-term dietary survey ever undertaken: the 121,700-participant Nurses’ Health Study, begun in 1976 by Harvard Medical School professor Frank Speizer, with dietary assessments supervised by Willett since 1980. The study isn’t just big: Willett carefully crafted it so that he and others could extract specific recommendations about food intake. Participants even surrender blood and toenail samples so that Willett can track absorption of trace elements and other nutrients. If a participant reports a major illness, such as heart attack or cancer, “we write for permission to obtain medical records for further details,” says Willett. To ensure that the data include both sexes and two generations, Willett and several colleagues also launched the Health Professionals Follow-Up Study, which includes 52,000 men, and the Nurses’ Health Study II, a survey of 116,000 younger women. In the past, nutritional scientists have largely relied on studies of animals, small groups of people, and/or petri-dish biochemistry that may not reflect the vagaries of human metabolism, although Willett uses such studies when he deems it appropriate. His access to a unique quarter-million-person pool of humans who carefully track both their diets and their health lends added credibility to his research. “When you put animal, metabolic, and epidemiological studies together and they all point in the same direction, you can be pretty confident about your conclusions,” Willett says * Adding a small bag of French fries (26 grams of carbohydrates) to your lunch is the equivalent of ingesting 6.5 teaspoons of refined sugar. The glycemic index is 67 (medium). The glycemic load is about 17 (medium). Potatoes put glucose into the bloodstream as fast as or faster than refined sugar. (To understand glycemic load and glycemic index, see “Good Carbs/Bad Carbs” on page 49.) * While soft-spoken and self-effacing in person, Willett isn’t shy about using this formidable database to take on the federal establishment. His Healthy Eating Pyramid differs radically from the Food Guide Pyramid pushed by the U.S. Department of Agriculture. “At best, the USDA pyramid offers wishy-washy, scientifically unfounded advice,” Willett argues in his book, Eat, Drink, and Be Healthy: The Harvard Medical School Guide to Healthy Eating. At worst, he adds, “the misinformation contributes to overweight, poor health, and unnecessary early deaths.” The numbers back him up. Men and women in Willett’s studies whose diets most closely paralleled the Healthy Eating Pyramid’s guidelines lowered their risk of major chronic disease by 20 percent and 11 percent respectively, according to an article published in the December 2002 issue of The American Journal of Clinical Nutrition. That compares with reduced risks of 11 percent and 3 percent for those whose diets most closely mirrored the USDA pyramid’s guidelines. “Nutrition used to be like religion. Everyone said, ‘I have the truth, everyone else is wrong,’ and there wasn’t much data to refute that,” says Willett. “Now we’re starting to have a real scientific basis for understanding what you should eat.” * Three four-inch pancakes (33 grams of carbohydrates) for breakfast with a quarter cup of syrup (52 grams of carbohydrates) is equivalent to eating 21 teaspoons of refined sugar. The glycemic index of the meal is about 65 (medium). The glycemic load for the pancakes is 27 (high) and 28 (high) for the syrup. * Willett says, the American public has been victimized by dodgy advice. Not only has obesity skyrocketed but “the incidence of heart disease is also not going down anymore. It has really stalled.” What happened? In Willett’s view, things began to go awry in the mid-1980s, when a National Institutes of Health conference decreed that to prevent heart disease, all Americans except children under 2 years old should reduce their fat intake from 40 percent to 30 percent of their total daily calories. The press touted the recommendation as revealed truth, and the USDA’s Food Guide Pyramid, released in 1992, reflects this view, calling for 6 to 11 servings of bread, cereal, rice, and pasta daily, while fats and oils are to be used “sparingly.” Too bad, says Willett. “The low-fat mantra has contributed to obesity. The nutrition community told people they had to worry only about counting fat grams. That encouraged the creation of thousands of low-fat products. I call it ‘the SnackWell revolution.’” Blithely consuming low-fat foods full of carbohydrates is a prescription for portliness, says Willett, adding that any farmer knows this. “If you pen up an animal and feed it grain, it will get fat. People are no different.” The problem with overeating refined carbohydrates such as white flour and sucrose (table sugar) is that amylase, an enzyme, quickly converts them into the simple sugar called glucose. That goads the pancreas to overproduce insulin, the substance that conducts glucose into the cells. But excessive sugar is toxic to cells, so after years of glucose and insulin overload, the cells can become insulin resistant and may no longer allow insulin to easily push glucose inside them. That keeps blood glucose levels high, forcing the pancreas to make even more insulin in a desperate attempt to jam the stuff through cell membranes. Willett likens the effect to an overworked, under maintained pump that eventually wears out. Type 2 diabetes can be one result, but Willett contends that insulin-resistant people who don’t develop full-blown diabetes still face significant health risks. Other researchers agree. Stanford endocrinologist Gerald Reaven coined the term Syndrome X to describe the constellation of health problems that spring from insulin resistance. Until the late 1980s, Reaven says, “the common scientific view was that insulin resistance only mattered if it led all the way to type 2 diabetes. Looking at the data, it’s clear that most people who are insulin resistant don’t get diabetes but are greatly at risk for coronary heart disease, hypertension, non-alcoholic-type liver disease, polycystic ovary syndrome, and several kinds of cancer.” WILLETT VS. ORNISH VS. ATKINS Walter Willett’s dietary recommendations are similar in many ways to those advanced by another doctor-nutritionist, Dean Ornish, who pioneered an ultralow-fat, near-vegetarian regime that has been shown to halt or reduce coronary blockage in most heart patients. Both Willett and Ornish emphasize whole grains, fruits, and vegetables, and both minimize animal proteins. But they part ways on fats: Willett recommends replacing saturated fats in the American diet with unsaturated ones, while Ornish suggests sharply cutting fat intake altogether, especially for those at risk for heart disease. “No one has shown that the kind of diet that Walter Willett recommends can reverse heart disease,” says Ornish. For his part, Willett insists that “replacing saturated fats with unsaturated fats is a safe, proven, and delicious way to cut the rates of heart disease.” He says the Lyon Diet Heart study, a French trial that tracked heart-attack survivors on an oil-rich Mediterranean diet versus those on the low-fat American Heart Association diet, showed a significant drop in second attacks for the Lyon group. Ornish responds that the drop in deaths in that study was most likely due to increasing heart-healthy omega-3 fats and decreasing intake of omega-6 fats, saturated fats, animal protein, and cholesterol, not to high overall consumption of fat. Ornish recommends that everyone consume three grams of omega-3 fats daily, either through eating fish or taking supplements. In contrast with both Willett and Ornish, the late Robert Atkins recommended a meat-intensive, protein-rich regime. “Studies at Duke University, the University of Cincinnati, and the University of Pennsylvania all show that people can lose significant weight, lower their triglycerides, and improve their HDL [high-density lipoprotein] cholesterol levels by consuming protein and limiting carbohydrates,” says Stuart Trager, an orthopedic surgeon who assumed the spokesman’s mantle for the diet after Atkins’s death in April 2003. Trager believes the real strength of the Atkins diet is that “it is something people are willing and able to do.” Willett concedes that Atkins “was really onto something. He believed, correctly, that most people can better control their weight by reducing the glycemic load of the diet than by other means. But there is evidence that the traditional Atkins diet, which is high in animal fat, is not optimal. There are benefits to having cereal in one’s diet. There is relief from constipation, and we do see [in the Nurses’ Health Study] some benefit for heart disease and diabetes. This is probably partially from the fiber in whole grains, and also partly from the other minerals and vitamins that come along with whole grains that are in short supply in many people’s diets.” While at first blush the three approaches seem sharply divergent, Trager sounds a conciliatory note. “No one has ever bothered to point out that we are compatriots on many points,” he says. All three nutritionists share an emphasis on reducing blood-sugar spikes by reducing the glycemic load. Moreover, all three condemn trans fats, white flour, and sugar. “There really is universal agreement that you should cut those things out of your diet,” Trager says. --Brad Lemley In the case of heart disease, Reaven says that high blood concentrations of insulin and glucose can damage the endothelium that lines coronary arteries and set the stage for the formation of plaques. “A big problem is the lack of drugs to treat this problem,” he adds. “A lot of doctors’ education comes from drug companies. They know about cholesterol because everyone is pushing their statin. They know about hypertension because there are multiple hypertensive drugs. But they know a lot less about insulin resistance and its consequences, and that’s unfortunate.” Syndrome X, also known as metabolic syndrome or insulin-resistance syndrome, is largely unknown to the public as well. While many people avoid cholesterol and fat-laden foods, few understand the threat posed by carbohydrate excess. That needs to change, says Willett. “Cholesterol is relevant, but the danger is overblown,” he says. “Syndrome X is the global public-health problem of the 21st century. Almost certainly the vast majority of Americans have a higher degree of insulin resistance than is optimal.” The Willett plan aims to even out the glucose roller coaster through an emphasis on foods with low glycemic loads—foods that convert to glucose slowly—like whole grains, plant oils, and vegetables. This keeps blood glucose levels relatively constant, sparing the pancreas overwork. Steady blood glucose also helps keep the appetite in check, which makes maintaining a healthy weight easier, says Willett. So instead of high carb, low fat, one might summarize the Willett plan’s directive as good carb, good fat. “People are being told to reduce fat and eat more carbohydrates. For many people, particularly overweight people with a high degree of insulin resistance, that produces exactly the opposite of what they need,” says Willett. Randomized trials, he says, show that people on low-fat diets generally lose two to four pounds after several weeks but then gain back the weight even while continuing the diet. “Most of them would be better off reducing carbs, switching to better carbs, and increasing their intake of healthy fats.” Willett, like virtually every other nutrition researcher, advises eating vegetables in abundance, consuming alcohol in moderation, and taking a daily multivitamin to cover nutritional gaps. He also touts fish as a source of protein and heart-protective n-3 fatty acids, which are also known as omega-3 acids. (Those who worry about mercury contamination in fish got some good news recently: In one study conducted in the Seychelles, a group of islands in the Indian Ocean, scientists from the University of Rochester Medical Center tracked pregnant women who ate an average of 12 fish meals a week, about 10 times the quantity of fish eaten by the average American. “We’ve found no evidence that the low levels of mercury in seafood are harmful,” said lead author Gary Myers. Moreover, various tests indicated that the women’s children suffered no adverse cognitive, behavioral, or neurological effects.) High on the list of food ingredients Willett counsels avoiding are hydrogenated fats, often referred to as trans fats, which are found in shortening, margarine, deep-fried foods, and packaged baked goods. That advice was controversial when Willett published a groundbreaking paper on the subject in 1991, but it has since become close to dogma. “Both controlled-feeding studies that have examined the effects of trans fat on blood cholesterol and epidemiological studies of trans-fat intake in relation to the risk of heart disease and diabetes indicate they are considerably worse than saturated fats,” he says. Daily exercise is essential, Willett adds, and he confirms the often-cited advice that walking is the best choice for many people. The Nurses’ Health Study revealed a “very strong link” between walking and protection against heart disease: Women who walked an average of three hours a week were 35 percent less likely to have a heart attack over an eight-year period than those who walked less. It may seem odd that Willett includes exercise in his Healthy Eating Pyramid, but he is adamant that exercise and diet cannot be teased apart. “It doesn’t have to be extreme. I run along the Charles for 25 minutes most mornings.” A half hour daily of moderate activity offers “impressive health benefits,” he says, but there is “added benefit for greater intensity for longer times.” Willett’s more iconoclastic conclusions include the heretical notion that soy—touted as a miracle food that fights cancer, obesity, and virtually every other human ill—may have “a dark side.” He points to a British study in which 48 women with suspicious breast lumps were randomly assigned to receive either no supplement or one containing soy isoflavones (a compound in soybeans molecularly similar to estrogen) for 14 days. Those taking the supplement showed substantially more cell growth in the tissue removed than the women who were not taking the soy. Another troubling study showed memory loss and other cognitive declines in elderly Japanese men in Hawaii who stuck to their traditional soy-based diet, as opposed to those who switched to a more of a Western diet. “In moderation, soy is fine,” says Willett. “Stuffed into everything, you could get into trouble.” And soy isoflavone supplements, he counsels, should be regarded as “totally untested new drugs.” Willett also counsels that dairy products—which supply concentrated calories and saturated fat—are not the best way to get calcium and that the recommended daily intake of 1,200 milligrams daily for adults over 50 appears to be more than what’s needed. His advice: Eat calcium-bearing vegetables, including leafy greens, take calcium supplements if you’re a woman, and exercise. “The evidence for physical activity being protective against fractures is huge,” he says. And he defends eggs. Although cholesterol fears have caused American per capita egg consumption to drop from 400 to 250 per year, “no research has ever shown that people who eat more eggs have more heart attacks than people who eat fewer eggs,” Willett says. A 2001 Kansas State University study identified a type of lecithin called phosphatidylcholine in eggs that interferes with cholesterol absorption, which may explain why many studies have found no association between egg intake and blood cholesterol level. If the breakfast menu option is a white-flour bagel or an egg fried in vegetable oil, says Willett, “the egg is the better choice.” * Having one-third of a 12-inch pepperoni pizza for dinner on the run? The cheese and crust amount to about 84 grams of carbohydrates, or the equivalent of wolfing down 21 teaspoons of sugar. The glycemic index of that meal is 60 (medium). The glycemic load is 51 (high). * Perhaps the most comprehensive studies Willett has assembled compare the health consequences of eating saturated versus unsaturated fat. The term saturated means that every available site along each fat molecule’s carbon chain is filled with a hydrogen atom; such fats—including butter and animal fat—are solids at room temperature. There are two types of unsaturated fats: monounsaturated fats such as olive oil, which are missing one pair of hydrogen atoms, and polyunsaturated fats such as soy, corn, and canola oils, which lack more than one pair. Both sorts are liquid at room temperature. Some researchers have questioned whether saturated fat is dangerous. In his book, The Cholesterol Myths: Exposing the Fallacy That Saturated Fat and Cholesterol Cause Heart Disease, Swedish physician Uffe Ravnskov asserts that as of 1998, 27 studies on diet and heart disease had been published regarding 34 groups of patients; in 30 of those groups investigators found no difference in animal fat consumption between those who had heart disease and those who did not. “Anyone who reads the literature in this field with an open mind soon discovers that the emperor has no clothes,” Ravnskov writes. Willett turns to his Nurses’ Health mega-study for the definitive word. “The amounts of specific fats did make a difference,” he says. “Women who ate more unsaturated fat instead of saturated fat had fewer heart problems.” Willett calculated that replacing 5 percent of saturated fat calories with unsaturated would cut the risk of heart attack or death from heart disease by 40 percent. Other studies—notably the French Lyon Diet Heart study, begun in 1988—show a similar correlation. A healthy diet plan is worthless if people won’t stick to it, and Susan Roberts, director of the energy metabolism laboratory at Tufts University, contends that Willett’s regimen is too severe. “Most people would say his recommendations are healthy but that other, less difficult diets are healthy too,” she says. Difficult is in the palate of the eater. The last half of Willett’s book aims to dispel any taint of Calvinism with recipes that verge on the sybaritic, including pork tenderloin with pistachio-gremolata crust, chicken enchilada casserole, and grilled salmon steaks with papaya-mint salsa. On the other hand, some resolve might be required to soldier through a few of the other dishes listed there, including hearty oat–wheat berry bread or the onion-crusted tofu-steak sandwich. But most people, Willett believes, can summon the willpower to substitute whole-wheat flour for white and plant oils for shortening or lard, and eat less sugar overall. “I think what I suggest is not severely restrictive, because it can be achieved mainly by substitution,” rather than slavishly following recipes, Willett says. In any case, “it does not mean you cannot eat any of those foods but rather that they should be de-emphasized.” So take heart. Even Willett has a little chocolate now and then. * GOOD CARBS/BAD CARBS The glycemic index (GI) is a way of measuring how quickly the carbohydrate in a given food raises the level of blood sugar. So eating a low-GI food causes a slow, mild rise, while the same quantity of carbohydrate in a high-GI food will trigger a faster, bigger rise. A GI of 55 or less is considered low, 56 to 69 is medium, and 70 or more is high. But the GI is of limited use in the real world of pears, pork, and pudding because it ignores how much of that food a person eats. A few years ago, Walter Willett pioneered the concept of the glycemic load (GL), a measurement that factors in the quantity of carbohydrates eaten in a single serving of a particular food. The carbohydrates in parsnips, for example, are quickly converted to glucose, so parsnips have a rather high index of 97, plus or minus 19 (the numbers are sometimes imprecise because they are based on feeding foods to test subjects and monitoring their blood-sugar response, which can vary for many reasons). But parsnips have a GL of just 12, because a single 80-gram serving contains a relatively small amount of carbohydrate. A GL of 10 or less is considered low, 11 to 19 is medium, and 20 or more is high. Consistently eating low-GL foods evens out blood-sugar peaks and valleys, which Willett says helps keep appetite and weight under control. Eating low-GL foods also reduces the risk of developing type 2 diabetes. When Willett says “good carbs,” he is essentially referring to fiber-rich, low-GL foods. Generally, whole grains have lower glycemic loads than refined grains. For example, a 150-gram serving of brown rice has a GL of 18, while the same serving of quick-cooking white rice has a GL of 29. Although the photographs in this story tally the “sugar equivalence” of the carbohydrates in various American foods, the glycemic index and glycemic load of each of these foods needs to be considered as well. The glycemic numbers accompanying the photographs in this article are from Janette Brand-Miller of the University of Sydney, based on a table published in the July 2002 issue of The American Journal of Clinical Nutrition. An adaptation of that table can be seen at diabetes.about.com/library/mendosagi/ngilists.htm. —B. L. 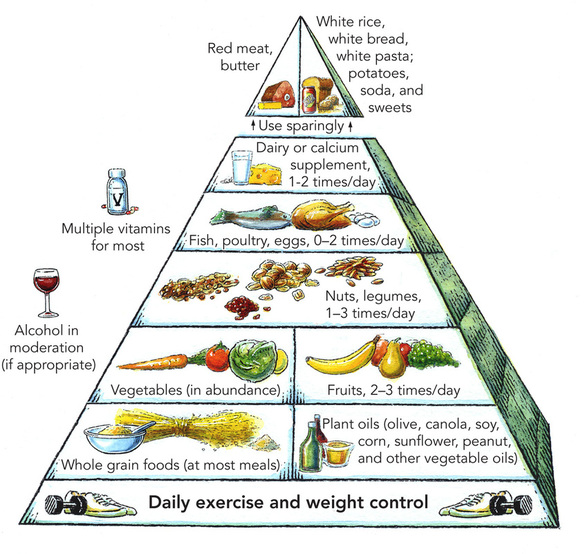 What science says you should eat. What science says you should eat.
Walter Willett finds it useful to present dietary information in pyramid form, with the broad base representing exercise and foods to emphasize and the small tip showing foods to avoid. “It’s simple,” he says. “It gives you a sense of priorities.” But he argues that the federally sanctioned USDA Food Guide Pyramid is deeply flawed. “The thing to keep in mind about the USDA pyramid is that it comes from the Department of Agriculture, the agency responsible for promoting American agriculture, not from agencies established to monitor and protect our health,” he says. Willett’s alternative Healthy Eating Pyramid draws a distinction between good and bad fats, between whole-grain and refined carbohydrates, and between healthy and problematic sources of protein. It also moves potatoes out of the vegetable category altogether. “Potatoes should be counted as starches. They are converted to glucose as fast or faster than pure table sugar,” he says. —B. L. Animal protein-rich diets could be as harmful to health as smokingPeople under 65 who eat a lot of meat, eggs and dairy are four times as likely to die from cancer or diabetes, study suggests
The study throws doubt on the long-term safety of the Atkins and Paleo diets, which are high in meat, eggs and other sources of animal protein. Photograph: Reuters A diet rich in meat, eggs, milk and cheese could be as harmful to health as smoking, according to a controversial study into the impact of protein consumption on longevity. High levels of dietary animal protein in people under 65 years of age was linked to a fourfold increase in their risk of death from cancer or diabetes, and almost double the risk of dying from any cause over an 18-year period, researchers found. However, nutrition experts have cautioned that it's too early to draw firm conclusions from the research. The overall harmful effects seen in the study were almost completely wiped out when the protein came from plant sources, such as beans and legumes, though cancer risk was still three times as high in middle-aged people who ate a protein-rich diet, compared with those on a low-protein diet. But whereas middle-aged people who consumed a lot of animal protein tended to die younger from cancer, diabetes and other diseases, the same diet seemed to protect people's health in old age. The findings emerged from a study of 6,381 people aged 50 and over who took part in the National Health and Nutrition Examination Survey (NHANES) which tracks a representative group of adults and children in the US. The study throws doubt on the long-term health effects of the popular Atkins and Paleo diets that are rich in protein. Instead, it suggests people should eat a low-protein diet until old age when they start to lose weight and become frail, and then boost the body's protein intake to stay healthy. In the over-65s, a high-protein diet cut the risk of death from any cause by 28%, and reduced cancer deaths by 60%, according to details of the study published in the journal Cell Metabolism. Valter Longo, director of the Longevity Institute at the University of Southern California, said that on the basis of the study and previous work, people should restrict themselves to no more than 0.8g of protein a day for every kilogram of body weight, equivalent to 48g for a 60kg person, and 64g for an 80kg person. "People need to switch to a diet where only around nine or ten percent of their calories come from protein, and the ideal sources are plant-based," Longo told the Guardian. "We are not saying go and do some crazy diet we came up with. If we are wrong, there is no harm done, but if we are right you are looking at an incredible effect that in general is about as bad as smoking." "Spend a couple of months looking at the labels on your food. There is a little bit of protein everywhere. If you eat breakfast, you might get 4g protein, but a piece of chicken for lunch may have 50g protein," said Longo, who skips lunch to control his calorie and protein intake. People who took part in the study consumed an average of 1,823 calories a day, with 51% coming from carbohydrates, 33% from fat, and 16% from protein, of which two thirds was animal protein. Longo divided them into three groups. The high-protein group got 20% or more of their calories from protein, the moderate group got 10 to 19% of their calories from protein, and the low group got less than 10% of calories from protein. Teasing out the health effects of individual nutrients is notoriously difficult. The apparently harmful effects of a high-protein diet might be down to one or more other substances in meat, or driven by lifestyle factors that are more common in regular red meat eaters versus vegetarians. Other factors can skew results too: a person on the study who got ill might have gone off their food, and seen a proportional rise in the amount of calories they get from protein. In that case, it would be the illness driving the diet, not the other way round. "I would urge general caution over observational studies, and particularly when looking at diet, given the difficulties of disentangling one nutrient or dietary component from another. You can get an association that might have some causal linkage or might not," said Peter Emery, head of nutrition and dietetics at King's College London. Gunter Kuhnle, a food nutrition scientist at Reading University, said it was wrong "and potentially even dangerous" to compare the effects of smoking with the effect of meat and cheese as the study does. "Sending out [press] statements such as this can damage the effectiveness of important public health messages. They can help to prevent sound health advice from getting through to the general public. The smoker thinks: 'why bother quitting smoking if my cheese and ham sandwich is just as bad for me?'" Heather Ohly at the European Centre for Environment and Human Health in Exeter said: "Smoking has been proven to be entirely bad for us, whereas meat and cheese can be consumed in moderation as part of a healthy diet, contributing to recommended intakes of many important nutrients." Most people in Britain eat more protein than they need. The British Dietetic Association recommends a daily intake of 45g and 55g of protein for the average woman and man respectively. But according to the British Nutrition Foundation the average protein intake per day is 88g and 64g for men and women. In a series of follow-up experiments, Longo looked at what might lie behind the apparently damaging effects of a high-protein diet on health in middle age. Blood tests on people in the study showed that levels of a growth hormone called IGF-1 rose and fell in line with protein intake. For those on a high protein diet, rises in IGF-1 steadily increased their cancer risk. Further tests on mice found that a high-protein diet led to more cancer and larger tumours than a low-protein diet. From Dr. Wayne Coghlan... In summary.... You can imagine a life without beer, pizza, and ice cream... but why should you? If you are invited to a backyard birthday barbeque don't be a self righteous food prude. Just generally eat such things sparingly. For the most part, eat more* fruits, veggies (in abundance), and whole grains. Eat less* meat (less red meat), dairy, and egg. Live culture yogurt is good. A daily vitamin is a good idea. Alcohol, if at all, in moderation. Be more active and less sedentary. Invigorating exercise regularly. What does more* mean? More than you are now. What does less* mean? Less than you are now. The Mediterranean Diet gets it pretty close. Please feel free to contact me [email protected], and www.drwaynecoghlan.com
Best Diets in 2023: Mediterranean Diet
Wins AgainKathleen Doheny January 03, 2023 It's officially 2023, and if history repeats, millions of Americans are likely vowing that this year will be one when they drop those unwanted pounds for good. After all, weight loss usually lands one of the top spots on New Year's resolution surveys. And just in time, there's guidance to pick the best plan. Released today are U.S. News & World Report's annual rankings of the best diet plans. Once again, the Mediterranean diet, which emphasizes fruits, vegetables, olive oil, and fish, got the top spot, as best diet overall. It's the sixth consecutive year for that win. But many other diets got top marks as well. This year, U.S. News, with the help of more than 30 nutritionists, doctors, and epidemiologists, ranked 24 diets in several categories to help people find a plan that meets their goals, whether it's finding the best weight loss diet, easiest one to follow, or plans for other goals, such as managing diabetes or heart disease. Two new categories were added: Best Diets for Bone & Joint Health and Best Family-Friendly Diets. In previous years, the publication ranked 40 diets. Even if a diet is no longer ranked, its profile with detailed information remains on the site. "Each year we ask ourselves what we can do better or differently next time," says Gretel Schueller, managing editor of health for U.S. News. When the publication got feedback from their experts this year, they had requests to consider sustainability of diets and whether they meet a busy family's needs, in addition to considering many other factors. This year's report ranks plans in 11 categories. The winners and the categories: Best Diets Overall After the Mediterranean diet, two others tied for second place:
WW, formerly known as Weight Watchers, got first place. The plan emphasizes not only weight loss but healthier eating and regular activity. The Points program, which assigns specific points to foods, with a daily Points budget, is more personalized than in the past.
The keto diet got first place. It's a high-fat, low-carb diet that aims to achieve weight loss through fat burning. Four others tied for second place:
DASH and Mediterranean are in a first-place tie, followed by the flexitarian diet. Best Family-Friendly Diets This category has a three-way tie: the flexitarian, Mediterranean, and TLC diets. Best Plant-Based Diets Mediterranean was first, then flexitarian and the MIND diet. The MIND diet combines the DASH and Mediterranean diets and focuses on "brain-healthy" foods. Easiest Diets to Follow Flexitarian and TLC tied for first, followed by a tie between DASH and Mediterranean. Best Diet Programs (formerly called commercial plans)
Response from Diet PlansRepresentatives from two plans that received mixed reviews in the rankings responded. Jenny Craig was ranked second for best diet program but much lower for family-friendly, landing at 22nd place of 24. "Our program is designed to address the needs of the individual through personalized experiences," Jenny Craig CEO Mandy Dowson says. "We have many families that participate in our program together but are still evaluated separately to determine appropriate individual goals." Its high ranking for best diet program reflects feedback from satisfied members, she says. Among advances will be the new Jenny Fresh program, a line of entrées prepared fresh and delivered to customers' doors. Atkins got second place for best fast weight loss but ranked near the bottom for best overall, best weight loss, diabetes, healthy eating, and heart health. In response, Colette Heimowitz, vice president of nutrition and education for Simply Good Foods, which makes Atkins's food products, says that low-carb eating approaches are a viable option for anyone today. "There are more than 130 independent, peer-reviewed published studies that show the efficacy and safety of low-carb eating," she says. "The studies have been conducted for several decades and counting." Expert PerspectiveSamantha Cassetty, a registered dietitian, nutritionist, and wellness expert in New York City and author of Sugar Shock, reviewed the report for WebMD. She was not involved in the rankings. "I think what this shows you is, the best diet overall is also the best for various conditions," she says. For instance, the Mediterranean, the number one overall, also got high ranking for diabetes, heart health, and bone and joint health, she points out. For consumers trying to lose weight: "If you see fast weight loss, that should be a red flag. A healthy diet for weight loss is one you can sustain," she says. She's not a fan of the programs with prepackaged foods. "It takes the guesswork out, but the portion sizes tend to be unsatisfying. They don't teach you how to deal with some of the challenges [such as realizing an 'ideal' portion size]." How to Use the ReportSchueller's advice: "Recognize that no diet fits everyone." When considering which plan to choose, she suggests thinking long-term. "Whatever we choose has to work in the long run," she says. Consumers should consider expenses, meal prep time, and whether the diet fits their lifestyle. Ideally, she says, the best diet "teaches you smart food preparation and how to make healthy choices, allows the flexibility to be social and eat with groups, whether family or friends." Before choosing a diet to follow, consult a medical professional for input on the decision, U.S. News cautions. Sources:U.S. News & World Report: "2023 Best Diet Rankings." Gretel Schueller, managing editor, health, U.S. News & World Report. Samantha Cassetty, registered dietitian, New York City. Mandy Dowson, CEO, Jenny Craig. Colette Heimowitz, vice president, nutrition and education, Simply Good Foods. Credits: Lead Image: iStock/Getty Images WebMD Health News © 2023 Cite this: Best Diets in 2023: Mediterranean DietWins Again - Medscape - Jan 03, 2023.
Mind & Brain » Scientific American Volume 313, Issue 3 » The Science of Health
Mediterranean Eating Habits Prove Good for the Brain A Mediterranean-style diet may slow memory loss, even if adopted late in life By Dina Fine Maron | Aug 18, 2015 http://www.scientificamerican.com/article/mediterranean-eating-habits-prove-good-for-the-brain/?WT.mc_id=SA_MB_20150902 Aleks Sennwald Whenever the fictional character Popeye the Sailor Man managed to down a can of spinach, the results were almost instantaneous: he gained superhuman strength. Devouring any solid object similarly did the trick for one of the X-Men. As we age and begin to struggle with memory problems, many of us would love to reach for an edible mental fix. Sadly, such supernatural effects remain fantastical. Yet making the right food choices may well yield more modest gains. A growing body of evidence suggests that adopting the Mediterranean diet, or one much like it, can help slow memory loss as people age. The diet's hallmarks include lots of fruits and vegetables and whole grains (as opposed to ultrarefined ones) and a moderate intake of fish, poultry and red wine. Dining mainly on single ingredients, such as pumpkin seeds or blueberries, however, will not do the trick. What is more, this diet approach appears to reap brain benefits even when adopted later in life—sometimes aiding cognition in as little as two years. “You will not be Superman or Superwoman,” says Miguel A. Martínez González, chair of the department of preventive medicine at the University of Navarra in Barcelona. “You can keep your cognitive abilities or even improve them slightly, but diet is not magic.” Those small gains, however, can be meaningful in day-to-day life. From Fork to Brain Scientists long believed that altering diet could not improve memory. But evidence to the contrary started to emerge about 10 years ago. For example, Nikolaos Scarmeas of Columbia University and his colleagues collected information about the dietary habits and health status of about 2,000 Medicare-eligible New Yorkers—typically in their mid-70s—over the course of four years on average. In 2006 the investigators reported that tighter adherence to a Mediterranean diet, which had previously been linked to a lower risk of cardiovascular disease, was associated with slower cognitive decline and a lower likelihood of acquiring Alzheimer's disease. Because the researchers merely observed dietary patterns and did not control them—as would be the case in a clinical trial—doubts lingered, however. It was still possible that the apparent brain benefit was the result of chance or some other trait common to folks who consistently follow a Mediterranean diet in the U.S., such as educational achievement or particular life choices. Seven years later researchers pinned down some answers. In 2013 Martínez González and his colleagues published findings on their massive PREDIMED study, an experiment that included almost 7,500 people in Spain. (PREDIMED stands for Prevention with Mediterranean Diet.) The investigators randomly assigned study subjects to one of two experimental groups. In the first, participants followed the Mediterranean diet with an additional helping of mixed nuts; in the second, they also adhered to the Mediterranean diet but were given additional extra virgin olive oil. (Researchers felt that providing extra nuts and oils at no cost to participants would guarantee that certain healthy fats were eaten in quantities large enough to have measurable effects on the study's outcomes.) The control group, against which the results of the experimental groups would be compared, was instructed generally on how to lose weight. Its members were given advice on eating vegetables, meat and high-fat dairy products that jibed with the Mediterranean diet, but they were discouraged from using olive oil for cooking and from consuming nuts. As expected, the results showed that either of the experimental Mediterranean diet options led to significantly better cardiovascular outcomes. But when the scientists tested cognition in a subset of study members, they also discovered that individuals in either of the Mediterranean diet groups performed better than the weight-instruction group in a battery of widely accepted cognitive tests. “This is surprising, of course,” Martínez González says. As intriguing as these findings are, they are still not conclusive; the researchers had not gathered any cognitive information at the beginning of the study. Therefore, the possibility remains that there was something different between the two experimental groups and the control group—beyond their diet interventions—that could account for the findings. Martínez González sought to quiet such criticisms with a new study his team published in July in JAMA Internal Medicine. Drawing from a group of more than 300 participants who were also part of PREDIMED but at a specific site with more financial resources, the researchers conducted baseline cognitive measurements and compared them with that same group's results four years later. On average, people were 67 years old at the start of the study. The newest findings, Martínez González says, are consistent with what he found in his earlier studies. These results are also not definitive, however, because this substudy was relatively small. Yet, he notes, it is the first time scientists have seen improvements in cognitive function from a randomized trial of the Mediterranean diet. Can Americans, whose standard diet and way of life are often substantially different from that of adults living in Spain, benefit from the approach? That remains to be seen. The normal diet of the people in the study's control group was still closer to a Mediterranean diet than that of most Americans, so they already had years of relatively healthy eating under their belts, which could have helped their overall health. But Martínez González believes that the diet might provide even greater benefits for Americans because they have so much more room for improvement. Still, nutrition expert Martha Morris of Rush University says, only a randomized trial in the U.S. can truly answer the question—something she hopes to spearhead in the coming years. Beyond Diet Proving that a particular cuisine affects cognitive health is one thing. Getting a lot of Americans to eat more fruits, vegetables, fish and olive oil is another matter altogether. Two major obstacles are cost and ingrained habits. For PREDIMED, study participants were supplied with expensive extra virgin olive oil and told how to prepare meals. “To transfer this knowledge to the American population, you can't just show them food items,” Martínez González says. “You have to show them how to shop for them, cook with them and prepare them to keep all the nutrients in line with the traditional Mediterranean diet.” The first step in the right direction, he says, would be for Americans to slash their consumption of red meats and use poultry instead. But that still leaves a lot of other steps to go before they are eating a Mediterranean diet. Adhering to the exact diet laid out in PREDIMED may not be the only way to gain cognitive benefits from food. In February, Morris and her colleagues published online a study recommending a modified diet largely consistent with the Mediterranean diet but one cheaper to adopt in the U.S. Morris's so-called MIND diet emphasizes green, leafy plant and whole grain consumption. Its staples include two veggie servings a day, two berry servings a week and, instead of the almost daily fish consumption required in the Mediterranean diet, fish only once a week. Morris found that even moderate adherence to the MIND diet for an average of 4.5 years appeared to reduce Alzheimer's risk compared with the Mediterranean and another diet. She and her colleagues judged that outcome by counting the number of cases of clinically diagnosed Alzheimer's among each group during the study period. (The comparison diets required stricter adherence to get the same cognitive benefit.) Better yet, the MIND diet may be more achievable for the average person's wallet and for American culture. In the bigger picture, this finding suggests that “people improving their diet can make a difference for their memory,” says Francine Grodstein, a professor focusing on healthy aging at Brigham and Women's Hospital in Boston and Harvard Medical School, who was not involved with the work. Why certain food choices might help the brain function better remains unclear. Perhaps these regimens' known cardiovascular benefits, which promote a good flow of blood and oxygen to the brain, are key. But other factors may be at work. Of course, questions about when these dietary changes need to happen or how diet stacks up against other factors, such as physical activity, sleep patterns and genetics also remain unanswered. Recently some researchers have begun broadening their focus beyond food alone. In the European Union, a multicountry randomized trial beginning this year is designed to provide further insights into how diet, exercise and better control of blood pressure could work together to promote brain health. (Hypertension is a leading cause of stroke, which can seriously harm mental processing.) Although the study will not allow scientists to pinpoint which factor offers the greatest benefit, it should give them a better understanding of how significant a role life changes can play. There is reason to be hopeful. A pilot study published in June in the Lancet found that making changes in diet and habits later in life can slow the course of cognitive decline. Scandinavian researchers divided a group of 1,260 people in Finland either to receive standard nutrition and diet advice or to follow a specified exercise plan and eat a modified Mediterranean diet—all while their blood pressure and other health indicators were monitored and, if necessary, treated. Subjects in the experimental group ended up doing significantly better on standard tests of cognition. “We could really see that [the intervention] can protect against or at least delay cognitive impairments,” says lead study author Miia Kivipelto, director of research and education at the geriatric clinic at the Karolinska Institute in Stockholm. Unexpectedly, she says, those changes were visible within just two years. And best of all, superpowers are not required. ABOUT THE AUTHOR(S) Dina Fine Maron is an associate editor at Scientific American. She focuses on medicine and health. This article was originally published with the title "Brain Food." Dr. Wayne Coghlan: ChiropractorMore support for the Mediterranean DietNot all vegan or plant-based diets are equally healthy By HENA PATEL and KIM ALLAN WILLIAMS SR. AUGUST 22, 2017 Move over, low-fat diets. More and more experts are recommending plant-based diets to reduce the risk of heart disease and other chronic conditions such as diabetes and cancer. But are all plant-based diets equally beneficial? And must they be all-or-none eating strategies, or is there a role for a semi-vegetarian or “flexitarian” approach? The term plant-based diet often conjures up images of vegetarian or vegan fare. But it really means a diet that emphasizes foods from plants — vegetables, fruits, grains, nuts, seeds, and the like — not one that necessarily excludes non-plant foods. The results of studies on the health effects of plant-based diets have varied widely, largely due to how these diets were defined. Some focused on vegetarian or vegan eating habits, others included some foods from animals. Notably, these studies tended to treat all plant foods equally, even though eating certain foods from plants, such as refined grains and sugar-sweetened beverages, is associated with a higher risk of developing diabetes or having a heart attack or stroke, while eating whole grains and produce are associated with lower risks. That’s why we were so interested to see the results of a recently published study performed by researchers at the Harvard T.H. Chan School of Public Health. Led by Ambika Satija, the team catalogued the diets of nearly 210,000 nurses and other health professionals based on their answers to food frequency questionnaires every two years for an average of 23 years. From these data, the researchers defined three versions of a plant-based diet: an overall plant-based diet that emphasizes the consumption of all plant foods and reduced the intake of animal foods; a healthful plant-based diet that emphasizes the intake of healthy whole grains, fruits, and vegetables; and an unhealthful plant-based diet that emphasizes the intake of less-healthy plant foods, such as refined grains. In addition to detailing their food choices, the study participants also recorded other lifestyle choices, health behaviors, and their medical histories. Over the course of the study, 8,631 participants developed coronary heart disease, which the researchers defined as a nonfatal heart attack or dying of heart disease. Those who followed an overall plant-based diet were slightly less likely (an 8 percent reduction) to have developed coronary heart disease than those who didn’t. But here’s where things get interesting. Those who followed a healthful plant-based diet had a substantial 25 percent lower risk of coronary heart disease, while those who followed an unhealthful plant-based diet had a substantial 32 percent increased risk. This study is certainly not the last word on the subject. As an observational study, it can’t prove cause and effect like a randomized trial can. And the diet data came from self reports, which aren’t always accurate at measuring an individual’s diet. However, these diet assessments were validated against multiple-week diet records and biomarkers. Overall, this work adds to the substantial evidence that a predominately plant-based diet reduces the risk of developing heart disease. It has two important take-home messages. One is that a plant-based diet is good for long-term health. The other is that not all plant-based diets are equally healthy. The kind that deserves to be highlighted in dietary recommendations is rich in fruits and vegetables, whole grains, and unsaturated fats, and contains minimal animal protein, refined carbohydrates, and harmful saturated and trans fats. In practice, this translates into eating mostly vegetables, fruits, whole grains, legumes, and soy products in their natural forms; sufficient “good fats,” such as those in fish or flax seeds, nuts, and other seeds; very few simple and refined carbohydrates; and little or no red meat, poultry, fish, eggs, and dairy. It also means choosing quality over quantity. Click here for a link to a description of the Mediterranean Diet.
Dear Gentle Reader:
Throughout my professional practice I have been chagrined at the wide variety of nutritional supplements to treat an even wider variety of maladies. The regulations to ensure purity and potency, as well as the efficacy of such products has been very slack allowing less scrupulous producers to flood the market with crap. The benefits for many if not most products are dubious at best. Such products are mostly harmless. At the very least they provide some entertainment and give people desperate to find some control over their health the illusion your are doing something beneficial. I suppose that can be understandable as, while modern Western health care has come a long way, it still falls short in many ways in it's availability, delivery, and despite the best of efforts, limitations. Some nutritional supplements however, carry a degree of toxicity and/or unfortunate cross reactions with other supplements and medications. And... people may do themselves preventable harm if they reject conventional and tested medically oriented treatments for otherwise bogus remedies. Trying to find good answers via the internet can be very challenging. There is much information that is based on conjecture, opinion, special knowledge, an effort to convince the consumer to buy a particular product, and plain misinformation. Much of it may be well intentioned, but it is still wrong. And while everyone may be entitled to an opinion, not every opinion is entitled. How then is one to know what products are helpful and at least meet some standard of purity and potency? Information from well know hospitals and universities is generally a good source (Mayo Clinic, Harvard Medical School). You may wish to see what research is available by using Google Scholar. Individual/independent sources should back up their claims by credible sources. To review: To help you toward your own informed decisions, here is a link to a respected source of research and information: Click on the logo below
Here are some links to other articles you may find interesting....
Best regards,
Dr. Wayne Coghlan www.drwaynecoghlan.com [email protected] I have been an advocate of "improve your posture - improve your life" for many years. Seems there is at least one other great thinker out there with the same idea and I present a few of her videos for your interest. Postural tone …. Emotional stress can produce physical injury…. Through postural stress and physical deterioration. Chiropractic avenue – when a person is not withstanding emotional stress well… it can affect the health in two ways… Physical posture…. The head comes forward…the shoulders droop…abdomen sags … mechanical stress on muscles in the neck and the joints and ligaments up and down the spine…this can lead to pain and arthritis …to resist the wearing of the tissues the muscles tighten leading to chronic strain….the muscles begin to change toward being tight and stringing instead of soft and fleshy… if you put your hands up to your shoulders and massage…and you feel those muscle knots.... those painful knots are part of the degenerative process. …Because of the stooped posture the breathing becomes shallow impairing lung function The second impact is muscle tension in the jaws and shoulders which compounds the physical strain… Cortisol levels rise in response to both emotional and physical stress… the body prepares to meet a threat that doesn’t come… the physical equivalent of walking uphill all day without the exercise. Yes… you can take some medication to relieve the pain… but what about the mechanism of injury? Unless you correct it…what is likely to continue happening? The process works in reverse too… postural deterioration can lead to emotional stress and deterioration. Alexander’s technique as an example. Alexander was a Shakespearean actor who suffered from nervous stage fright ( http://en.wikipedia.org/wiki/Alexander_technique). He found that when he consciously maintained impeccable poise and posture, his nerves settled, and curiously, his intonation and ability to project improved... as did several other health issues. He observed and postulated that many people develop inappropriate patterns of posture and movement and by correcting them, the person could often relieve the stress on their bodies as well as emotions. Own example…Give me a good slouch….feel your lungs…the energy in your neck and shoulders… the energy within your psyche… feeling happy? Over time the joints get pulled out of alignment….the muscles knotted up and the nervous system distressed. Good idea to see your friendly neighbourhood chiropractor! Yes! Social stress… The world reflects what we show it. Now a sit up tall… feel the difference… Lungs… shoulder…. Confidence. Published on Oct 1, 2012 Body language affects how others see us, but it may also change how we see ourselves. Social psychologist Amy Cuddy shows how "power posing" -- standing in a posture of confidence, even when we don't feel confident -- can affect testosterone and cortisol levels in the brain, and might even have an impact on our chances for success. Watch more talks at http://www.ted.com Dr. Wayne Coghlan: ChiropractorWeight LossWeighing in on Weight Loss There is much talk currently about regulating the diet/weight loss industry. I will leave that up to the reader to opine on the dangers, merits, and extent that Big Brother ought to protect the public from itself. However, as with many things in life, BUYER BEWARE. Keeping one's weight under control is important to promote a longer and healthier life. The number one indicator of adult onset disease is excess body weight. Weight loss, however, is a very challenging thing for most people to manage and sustain. Many people are desperate to find a better answer and .... in a free society there are those entrepreneurs who will take advantage of persons vulnerable, if not desperate. BUYER BEWARE. I recall a review of weight loss centres and their long term effectiveness. The research supported that for people who did adhere to their program, they were successful in temporarily losing weight. The problem came when the people stopped the program....over 90% regained and even exceeded their former weight. This was largely due to people not assuming personal responsibility for their weight management, and not successfully resolving their cultural, lifestyle and/or psychological needs that promoted weight gain. It doesn't take much to pack on the pounds...Remember, one hundred extra calories a day, that's one chocolate chip cookie, adds up to one pound a month! And yet.. one hundred calories a day less translates to a 1 lb weight loss per month. People who, over the long term, do succeed in managing their weight, are those who generally decide that they no longer wish to lose weight, they want to lose weight, and they will do what it takes to make it happen. I respect very much that this is easier to say than do. If such issues were simple, weight management would be less significant problem. ... Hmmm... I will amend that to state that the solution is mathematically simple... and yet obvious a challenge for many if not most people. I have over 24 years of professional experience in addition to eight plus years of post secondary education in health sciences. I have explored many and offered a few weight loss programs. Ultimately, there are two methods that are proven successful in losing weight. The first is to eat less and be more active. The second is to be more active and eat less. ANY weight loss program is a variation of those two themes. For some, surgical solutions may be the only truly effective solution, and yet they are still successful only because they force the person to cut calories. Any weight loss program that offers a quick fix for a lifelong problem, or is not based upon the simple mathematics of calories in (diet) vs. calories out (activity), is misleading you. A goal of losing one pound a week is considered reasonable....anything faster is dangerous and likely not sustainable. BUYER BEWARE. I will, respectfully suggest, that the most powerful idea about weight loss is TO STOP GAINING WEIGHT. We do that by using all the tricks we can. Eat less, of course, use a smaller plate. Take smaller portions. Stop eating when you are 80% satisfied. Don't buy junk food to keep in the house. Be more active, of course. Park at the far end of the parking lot. Take the stairs. Take a walk in the evening when you are waiting for your favourite show to start. Once you have stopped gaining weight, it takes very little adjustment to eat just 100 calories a day less. A 100 calorie a day deficit translates to about a pound a month. It's that simple... Do consider a new way of eating.. the Mediterranean Diet. And also review The French Paradox and What Science Says You Should Eat. Do take a look at Managing the Munchies! If you have and questions or comments, please connect with me via email at [email protected] and review my website at www.drwaynecoghlan.com Best regards, Dr. Wayne Coghlan Chiropractor.
Click to set custom HTML
Dr. Wayne Coghlan, Chiropractor, locum tenens, Ontario, Mississauga, Counselling Psychology, Anger management, Collingwood, Mississauga, drwaynecoghlan.com, www.drwaynecoghlan.com A variety of nonsense about stuff that maybe google will pick up on and please disregard this section. www.drwaynecoghlan.com, drwaynecoghlan.com, drwaynecoghlan.blogspot.com, https://www.facebook.com/DrWayneCoghlan
A very well done video that demonstrates the simple truth. If you want to be healthy, get and keep moving.....
Texting can put 60 pounds of pressure on your spine!
We are seeing more young people showing up with injuries to the spine (neck, shoulders, back) that were more typical of older adults and the main reason is from use of hand held electronic devices such cell phones and tablets. The study points out that the average adult human head weighs between 10 and 12 pounds when in the upright or neutral position, but due to gravitational pull, the cranium becomes heavier the more you bend your neck. Bending your head and neck forward, as when looking down at your cell phone when texting, creates a progressively increasing load on the cervical spine. As such, tilting your head a mere 15 degrees puts an added 27 pounds of pressure on your spine; a tilt of 30 degrees is equal to an extra 40 pounds of pressure, while a 45-degree tilt is akin to 49 pounds. At a 60-degree angle while texting puts 60 pounds of pressure on your cervical spine (the section of the spine situated just above the shoulders).
his can be demonstrated by holding something such as a baseball bat by the end. When the bat is held vertically the hand and arm just have to carry the load of the bat. If you then tip the bat toward the horizontal, the load on your hand and arm rapidly increases. Now try holding that load for a few minutes.
And since the typical person apparently spends an average of between two and four hours each day sending and receiving texts that translates into a whole lot of load on the muscles and joints of the neck and shoulders... and even the lower back. But wait, it gets worse: Loss of the natural curve of the cervical spine leads to incrementally increased stresses about the cervical spine. These stresses may lead to early wear, tear, degeneration and possibly surgeries. Click here for a discussion about the dangers of sustain loading of the spine and progressive deterioration. Bad posture has been linked to all manner of medical maladies, including headaches and neurological problems, along with depression, constipation and even heart disease. All of a sudden, texting your appetizer order to friends while running late doesn’t seem so important, right? Of course the problem is not limited to use of cell phones. We see the same issues from poor posture habits at the computer or other work stations. And from habits such as reading a book while resting it on your lap and bringing your eyes toward the book, instead of the book toward your eyes. And, who doesn't know the little old lady with the chronic neck pain, yet hunched over her knitting?
The good news is that most of those backaches can be remedied by the simplest of solutions: Stand up straighter. If you’re gradually feeling back pain, you might want to rethink your current texting habits.
The study defines correct posture as “ears aligned with the shoulders and the ‘angel wings’ or the shoulder blades, retracted.” While it is nearly impossible to avoid the technologies that cause these issues, individuals should make an effort to look at their phones with a neutral spine and to avoid spending hours each day hunched over. Dr. Wayne Coghlan can help you understand the cause of your headaches, neck and upper back and lower back pain and find long term relief.
___________________________________________________________________________________________________________________
There is a good argument that your posture can affect everything from your physical health to emotional health to social health to how much money you can make in your career. EXPLORE HERE!
___________________________________________________________________________________________________________________
Evidence Based Chiropractic
Pran Manga and Low Back Pain Pran Magna graduated from the University of Toronto with a PhD in economics in 1970. Since 1977 he has been a Full Professor at the Telfer School of Management at the University of Ottawa, where he teaches ethics, health economics, and globalization. He is also the director of the Masters Program in Health Administration. ••••• In 1993, the Ministry of Health, Government of Ontario, CANADA, commissioned Dr. Pran Manga and colleagues to evaluate the effectiveness and cost-effectiveness of chiropractic management of low-back pain. This project was undertaken because:
The Effectiveness and Cost-Effectiveness of Chiropractic Management of Low-Back Pain The last 15 pages of the book are a bibliography that contains approximately 400 citations. In the beginning of the book, Dr. Manga writes and signs a letter to: The Honourable Ruth Grier, Minister of Health, Ministry of Health, Government of Ontario, Toronto, Ontario, CAN. Pertaining to his booking regarding chiropractic and low back pain, his letter states: “We are very pleased to enclose our final report on the ‘The Effectiveness and Cost-Effectiveness of Chiropractic Management of Low-Back Pain’. It is rather voluminous testimony to the extensive and growing literature and clinical research in this area.” “In these times of severe fiscal constraints, we commend the Ministry of Health for funding much needed research in this increasingly important area, and we encourage further research pertinent to the consumer and provide surveys we recommend in the report. The potential for major gains in effectiveness and cost-savings is very significant. Our recommended reforms are all consistent with and promote the health care objectives of the Government of Ontario.” The EXECUTIVE SUMMARY of Dr. Manga’s book includes these points: [I added the bold emphasis] INTRODUCTION The serious fiscal crisis of all governments in Canada is compelling them to contain and reduce health care costs. It has brought a new and unprecedented emphasis on evidence-based allocation of resources, with an overriding objective of improving the cost-effectiveness of health care services. The area of low-back pain (LBP) offers governments and the private sector an excellent opportunity to attain the twin goals of greater cost-effectiveness and a major reduction in health care costs. Today LBP has become one of the most costly causes of illness and disability in Canada – a phenomenon which does not appear to be generally appreciated or understood in medical and government circles in Canada. Studies on the prevalence and incidence of LBP suggest that it is ubiquitous, probably the leading cause of disability and morbidity in middle-aged persons, and by far the most expensive source of workers’ compensation costs in Ontario – as indeed in most other jurisdictions. Much of the treatment of LBP appears to be inefficient. Evidence from Canada, the USA, the UK and elsewhere shows that there are conflicting methods of treatment, many with little – if any scientific evidence of effectiveness, and very high costs of treatment. Despite this, levels of disability from LBP are increasing. In the Province of Ontario, LBP is managed mostly by physicians and chiropractors, with physiotherapists also playing a significant role. While medical services are fully insured under Medicare, chiropractic care services are only partially covered. LBP patients incur the highest out-of-pocket expenses for chiropractic services. Virtually, no out-of-pocket expenses are incurred for medical treatment, with the exception of drugs, and out-of-pocket expenses incurred for physiotherapy services fall somewhere in between the two. Medical physicians, chiropractors, physiotherapists and an assortment of other professionals together offer about thirty-six therapeutic modalities for the treatment of LBP. In this study we focused principally on the effectiveness and cost effectiveness of chiropractic and medical management of LBP. FINDINGS
This report by Dr. Manga and colleagues assesses the most appropriate use of available health care resources for the management of low back pain. The report overwhelmingly supported the efficacy, safety, scientific validity and cost-effectiveness of chiropractic for low back pain. ••••• In 1998, Dr. Manga and colleague Doug Angus updated their original Manga Report with (2): Enhanced Chiropractic Coverage Under OHIP as a Means of Reducing Health Care Costs: Attaining Better Health Outcomes and Achieving Equitable Access to Health Services This document consists of 70 pages and 59 references. Their Executive Summary includes these Key Points:
Musculoskeletal disorders are also among the most important reasons for activity limitations and short-term disability. They rank first in prevalence in chronic health problems and first as a cause of long-term disability. Musculoskeletal disorders rank first as a reason for consultation with a health professional in Ontario, and rank second as a reason for the use of prescription and non-prescription drugs. There is considerable empirical support for the cost-effectiveness and the safety of chiropractic management of musculoskeletal disorders. This means that chiropractic care can bring about improved health outcomes at a lower cost.
Four out of five patients of chiropractors have had their problems for more than six months and have typically had medical and/or physiotherapy care before their visit to the chiropractor. The evidence is that chiropractic services should be frontline services for many NMS disorders rather than the default system of care when all else fails, as it seems to be for many patients. ••••• In 2000, Dr. Manga published an article in the Journal of Manipulative and Physiological Therapeutics, titled (3): Economic case for the integration of chiropractic services into the health care system In this article Dr. Magna states: “The role and position of chiropractic care in the health care system must be transformed from being alternative and separate to alternative and mainstream. This transformation requires that chiropractic services become integrated in the many health care delivery organizations that collectively constitute the health care system. There is solid and impressive economic and related justification for the desired integration.” “Chiropractic care is a cost-effective alternative to the management of neuromusculoskeletal conditions by other professions. It is also safer and increasingly accepted by the public, as reflected in the growing use and high patient retention rates. There is much and repeated evidence that patients prefer chiropractic care over other forms of care for the more common musculoskeletal conditions.” “The public interest will be well served by this transformation.” “Musculoskeletal disorders and injuries are the second and third most costly categories of health problems in economic burden-of-illness studies. They rank first as a cause in the prevalence of chronic health problems and long-term disability and rank at the top for activity limitations and short-term disability. They rank first as a reason for consultation with a health professional and second as a reason for the use of prescription and nonprescription drugs.” “These conditions are more prevalent among the poor, lower- middle income groups, and the elderly, yet those are precisely the groups that make the least use of chiropractic care for reasons of inadequate insurance coverage.” “The integration of chiropractic care into the health care system should serve to reduce health care costs, improve accessibility to needed care, and improve health outcomes.” ••••• In 2007, Dr. Manga was a co-author of a study also published in the Journal of Manipulative and Physiological Therapeutics, titled (4): Chiropractic care of musculoskeletal disorders in a unique population within Canadian community health centers In this study Dr. Magna and colleagues followed and assessed 259 patients with musculoskeletal complaints before and after a 12-week treatment period. Outcomes were assessed with:
“Clinically important and statistically significant positive changes were observed for all outcomes [with chiropractic care].” “No adverse events were reported.” “Patients of low socioeconomic status face barriers to accessing chiropractic services. This study suggests that chiropractic care reduces pain and disability as well as improves general health status in patients with musculoskeletal conditions.” To restate, this study found that a 12-week treatment with chiropractic in patients with musculoskeletal complaints resulted in statistically significant improvements in pain, in neck and back disability, and in general health status. ••••• In 2008, Dr. Manga was a co-author of another study published in the journal Explore (NY), [which is PubMed Indexed] titled (5): Developing integrative primary healthcare delivery: Adding a chiropractor to the team In this study Dr. Magna and colleagues sought to investigate the effect of integrating chiropractic on the attitudes of providers of healthcare teams. Two multidisciplinary healthcare teams at two community health centers in Ottawa, Ontario, CAN, participated in the study. The study lasted for 18 months. The health centers consisted of physicians, nurse practitioners, and degree-trained nurses. A chiropractor was introduced into each of the two healthcare teams. A quantitative questionnaire assessed providers’ opinions, experiences with collaboration, and perceptions of chiropractic care. Focus groups were used to encourage providers to communicate their experiences and perceptions of the integration and of chiropractic. The authors state: “Twelve providers were followed for the full 18 months of integration. The providers expressed increased willingness to trust the chiropractors in shared care. Questions regarding the legitimacy and effectiveness of chiropractic became increasingly positive by study end.” “This project has demonstrated the successful integration of chiropractors into primary healthcare teams.” This is one of the first and most unique assessments of the integration of traditional medical practice with chiropractic in an effort to create a workable and superior healthcare team. The positive outcome should be a model for continuing these efforts with the patient’s best welfare in mind. ••••• As closing note, on October 29, 1993, the newspaper USA TODAY published a follow-up to the original Manga Report, stating: A study, “done by a team of Canadian health economists commissioned and funded by the Ontario Ministry of Health – is based on an extensive review of international medical literature, as well as interviews with researchers, practitioners and patients.” “The best clinical studies show that spinal manipulation by chiropractors is more effective, safer and more cost-effective than other treatments for low-back pain.” “Chiropractors could save [Ontario, CAN, Health Ministry] hundreds of millions of dollars a year.” “Many medical therapies [for low back pain] are of questionable validity or are inadequate, and some are unsafe and even cause complications.” There is “good empirical evidence patients are very satisfied” with chiropractors and “considerably less satisfied with physician management” of low back pain. “Many [patients] pay out-of-pocket for chiropractor bills not covered by insurance; they wouldn’t if it didn’t help.” Manga states “I did not talk to a single chiropractor or person working for them, and they [chiropractors] did not know the study was being done.” The Manga Report “seems so positive one can’t help but wonder: does he have some personal interest in giving chiropractors a boost? ‘My interest is serving the public interest,’ Magna responds. ‘It’s not personal, and not family-related. If anything, I have many (medical) doctor in my family.’” Magna “simply believes his findings. ‘The evidence is overpowering.’” Magna states “I think [medical] doctors do know chiropractors are better and more effective for back pain.” CONCLUDING REMARKS The Manga Reports and journal articles are incredibly supportive of the perspective shared by the doctor sending you this letter. A thorough review of international literature shows that chiropractic is significantly superior to other approaches in the treatment of low back pain. Chiropractic care for the relief of low back pain is effective, cost effective, extremely safe, has extremely high levels of patient satisfaction, and could save hundreds of millions of dollars in Canada and undoubtedly billions of dollars in the United States. Primary research shows that chiropractic care for low back pain provides not only symptom relief but also reduces disability. Primary research also shows that integrating chiropractic into established medical practices remains impressive and well accepted by other health care providers. •••••••••• The Chiropractic Impact Report™ is a monthly publication by myself, Dan Murphy, DC. I am a 1978 graduate of Western States Chiropractic College in Portland, OR. I have managed about 10,000 whiplash-injury cases. In the past 32 years, I have taught more than 500 12-hour post graduate continuing education classes pertaining to whiplash and spinal trauma, including 21 years of coordinating a year-long certification program in spine trauma, certified through the International Chiropractic Association. Additionally, I am board certified in chiropractic orthopedics (DABCO), and I am on the faculty at Life Chiropractic College West in Hayward, CA (28 years). The purpose of The Chiropractic Impact Report™ is to keep you updated as to relevant academic concepts pertaining to whiplash-injured patients. The hope is that the information is useful in terms of enhanced understanding, as well as helping the personal injury attorney deal with insurance claim adjusters and adverse medical experts. The chiropractor sending you this Report is well versed and trained in these concepts, and can be a valuable asset in personal injury cases in terms of both academics and treatment. Additionally, these expert chiropractors have access to a monthly phone consultation with me to discuss any pertinent issues that they may be facing on a particular case. I hope that you find this Report and the referring chiropractor a valuable resource. Sincerely, Daniel J. Murphy DC, DABCO REFERENCES
Manga Report - The effectiveness and cost-effectiveness of Chiropractic Management of Low-back pain Executive Summary The Manga Report represents the largest existing analysis of scientific Literature on low-back pain to date. It has drawn national attention for the support of chiropractic treatment of low-back pain. This unbiased independent study commissioned by the Ontario Ministry of Health shows that chiropractic treatment is cost-effective, safe, has a high rate of patient satisfaction, and is more effective than medical treatment for low-back pain. The Manga Report also recommends that the management of low-back pain be moved from Medical Doctors to Doctors of Chiropractic and that hospital privileges be extended to D.C.s. This is a summarization of the findings of the Manga Report. INTRODUCTION The serious fiscal crisis of all governments in Canada is compelling them to contain and reduce health care costs. It has brought a new and unprecedented emphasis on evidence-based allocation of resources, with an overriding objective of improving the cost-effectiveness of health care services. The area of low-back pain (LBP) offers governments and the private sector an excellent opportunity to attain the twin goals of greater cost-effectiveness and a major reduction in health care costs. Today LBP has become one of the most costly causes of illness and disability in Canada – a phenomenon which does not appear to be generally appreciated or understood in medical and government circles in Canada. Studies on the prevalence and incidence of LBP suggest that it is ubiquitous, probably the leading cause of disability and morbidity in middle-aged persons, and by far the most expensive source of workers’ compensation costs in Ontario – as indeed in most other jurisdictions. Much of the treatment of LBP appears to be inefficient. Evidence from Canada, the USA, the UK and elsewhere shows that there are conflicting methods of treatment, many with little – if any – scientific evidence of effectiveness, and very high costs of treatment. Despite this, levels of disability from LBP are increasing. In the Province of Ontario LBP is managed mostly by physicians and Chiropractors, with physiotherapists also playing a significant role. While medical services are fully insured under Medicare, chiropractic care services are only partially covered. LBP patients incur the highest out-of-pocket expenses incurred for physiotherapy services fall somewhere in between the two. Physicians, chiropractors, physiotherapists and an assortment of other professionals together offer about thirty-six therapeutic modalities for the treatment of LBP. In this study, we focused principally on the effectiveness and cost-effectiveness of chiropractic and medical management of LBP. FINDINGS F1. On the evidence, particularly the most scientifically valid clinical studies, spinal manipulation applied by chiropractors is alternative treatments for LBP. Many medical therapies are of questionable validity or are clearly inadequate. F2. There is no clinical or case-control study that demonstrates or even implies that chiropractic spinal manipulation is unsafe in the treatment of low-back pain. Some medical treatments are equally safe, but others are unsafe and generate iatrogenic complication for LBP patients. Our reading of the literature suggests that chiropractic manipulation is safer than medical management of low-back pain. F3. While it is prudent to call for even further clinical evidence of the effectiveness and efficacy of chiropractic management of LBP, what the literature revealed to us is the much greater need for clinical evidence of the validity of medical management of LBP. Indeed, several existing medical therapies of LBP are generally contraindicated on the basis of the existing clinical trials. There is also some evidence in the literature to suggest that spinal manipulations are less safe and less effective when performed by non-chiropractic professionals. F4. There is overwhelming body of evidence indicating that chiropractic management of low-back pain is more cost-effective than medical management. We reviewed numerous studies that range form very very persuasive to convincing in support of this conclusion. The lack of any convincing argument or evidence to the contrary must be noted and is significant to us in forming our conclusions and recommendations. The evidence includes studies showing lower chiropractic costs for the same diagnosis and episodic need for care. F5. There would be highly significant cost savings if more management of LBP was transferred from physicians to chiropractors. Evidence form Canada and other countries suggests potential savings of many hundreds of millions annually. The literature clearly and consistently shows that the major savings from chiropractic management come from fewer and lower costs of auxiliary services, much fewer hospitalizations, and a highly significant reduction in chronic problems, as well as in levels and duration of disability. Workers’ Compensation studies report that injured workers with the same specific diagnosis of LBP returned to work much sooner when treated by chiropractors than by physicians. This leads to very significant reductions in direct and indirect costs. F6. There is good empirical evidence that patients are very satisfied with chiropractic management of LBP and considerably less satisfied with physician management. Patient satisfaction is an important health outcome indicator and adds further weight to the clinical and health economic results favouring chiropractic management of LBP. F7. Despite official medical disapproval and economic disincentive to patients (higher private out-of-pocket cost), the use of chiropractic has grown steadily over the years. Chiropractors are now accepted as a legitimate healing profession by the public and an increasing number of physicians. F8. In our view, the constellation of the evidence of:
RECOMMENDATIONS Our recommendations for reform include the following: R1. Current policy discourages the utilization of chiropractic services for the management of LBP. There should be a shift in policy to encourage and prefer chiropractic services for most patients with LBP. R2. Chiropractic services should be fully insured under the Ontario Health Insurance Plan, removing the economic disincentive for patients and referring health providers. This one step will bring a shift from medical to chiropractic management that can be expected to lead to very significant savings in health care expenditure, and even larger savings if a more comprehensive view of the economic costs of low-back pain is taken. R3. Chiropractic services should be fully integrated into the health care system. Because of the high incidence and cost of LBP, hospitals, managed health care groups (community health centres, comprehensive health organizations and health service organizations) and long-term care facilities should employ chiropractors on a full-time and/or part-time basis. Additionally such organizations should be encouraged to refer patients to chiropractors. R4. Chiropractors should be employed by tertiary hospitals in Ontario. Hospitals already employ chiropractic in the United States with good effect. Similar recommendations have been made recently by government inquiries in Australia and Sweden, and following government funded research in the U.K. and other countries. Unnecessary or failed surgery is not only costly but also represents low quality care. The opportunity for consultation, second opinion and wider treatment options are significant advantages we foresee from this initiative which has been employed with success in a clinical research setting at the University Hospital, Saskatoon. R5. Hospital privileges should be extended to all chiropractors for the purposes of treatment of their own patients who have been hospitalized for other reasons, and for access to diagnostic facilities relevant to their scope of practice and patients’ needs. R6. Chiropractors should have access to all pertinent patient records and tests from hospitals, physicians, and other health care professionals upon the consent of their patients. Access should be given upon the request of chiropractors or their patients. R7. Since low-back pain is of such significant concern to workers’ compensation, chiropractors should be engaged at a senior level by Workers’ Compensation Board to assess policy, procedures and treatment of workers with back injuries. This should be on an interdisciplinary basis with other professional, technical and managerial staff so that there is early development of more constructive relationships between chiropractors, physicians, physiotherapists and Board staff and consultants. A very good case can be made for making chiropractors the gate keepers for management of low-back pain in the workers’ compensation system in Ontario. R8. The government should make the requisite research funds and resources available for further clinical evaluation of chiropractic management of LBP, and for further socio-economic and policy research concerning the management of LBP generally. Such research should include surveys to obtain a better understanding of patients’ choices, attitudes and knowledge of treatments with respect to LBP. The objective of these surveys should be better information for health policy, program planning and consumer education purposes. R9. Chiropractic education in Ontario should be in the multidisciplinary atmosphere of a university with appropriate public funding. Chiropractic is the only regulated health profession in Ontario without public funding for education at present, and it works against the best interests of the health care system for chiropractors to be educated in relative isolation from other health science students. R10. Finally, the government should take all reasonable steps to actively encourage cooperation between providers, particularly the chiropractic, medical and physiotherapy professions. Lack of cooperation has been a major factor in the current inefficient management of LBP. Better cooperation is important if the government is to capture the large potential savings in question and, it should be noted, is desired by an increasing number of individuals within each of the professions. http://www.bcchiro.com/bcca/publications-and-resources/research-studies.html Research Studies Independent research shows that chiropractic is one of the most underutilized yet effective health care options available.
Dr. Wayne Coghlan,
Why Chiropractic? It's Re-Evolutionary! Here are some of the most common reasons why more than 4 million Canadians visit a chiropractor each year:
And just as the Re-Evolutionary graphic just above illustrates, many of these conditions develop from everyday wear and tear and strain. Back health is important The body’s information highway – your nervous system – is protected by the spine. The nervous system travels out between the vertebrae or joints of the spine to carry messages from the brain to every corner of your body. Stress and strain on the vertebrae can put pressure on the nerves in the affected area. That is why a problem with your spine can have far-reaching effects causing symptoms such as arm or leg pain. The word “chiropractic” comes from ancient Greek and means “done by hand.” Adjustment of the joints of the body has been used in the healing arts for many centuries and is at the heart of modern chiropractic care. Chiropractors are specialists in manual adjustment of the vertebrae of the spine and other joints of the body. Adjustment helps relieve pain and restore normal functioning to the joints and supporting muscles and ligaments – so you can enjoy your everyday activities again as quickly as possible. Your chiropractor will recommend a course of treatment specific to you that may also include mobilization of the joints, ultrasound, low intensity laser therapy, acoustic shockwave therapy, muscle release techniques, muscle stimulation and therapeutic exercises. Chiropractors are also trained to provide nutritional counselling, and recommend rehabilitation and injury prevention strategies. I also work with you to determine what situations may be causing your body stress and find strategies to overcome them, such as postural correction and computer use. When to consider chiropractic care If aching joints and muscle pain are affecting your ability to get through the day and keeping you away from your favourite activities, consider chiropractic care. Work, accidents, sports injuries, household chores, even the stress of daily living can cause painful joint and back problems. Even if you do not have painful symptoms, chiropractic care can help you maintain healthy spine, joint function, and support your healthy lifestyle. Benefits of chiropractic care Chiropractic treatment is skilled, hands-on health care that relieves pain and helps your body be its best. Here are some of the ways it can help you.
Be sure to visit Frequently Asked Questions for more information If you have any immediate questions, please contact me at [email protected] Dr. Wayne Coghlan: ChiropractorHonest Doc! ! Wasn't doing anything!"Honest, Doc! I wasn't doing anything!" We hear this one a lot from patients who limp, crawl, or are carried into our office. Every year, millions of people suffer sudden back or neck pain from no apparent injury. "It usually goes away in a couple of days, or if I take aspirin, so why should I worry?" Every time you overdo, there's a small amount of damage done to your spine. Vertebra (the bones of the spine) can slip out of position or move improperly as muscles pull. In a few days the muscles heal, the pain goes away, and the vertebrae stay out of place, creating a chronic but unfelt vertebral subluxation. This causes pressure on the nerves and can lead to fixation (a sticking together - seized joints) of two or more vertebrae. When vertebrae are fixated, the fluid in the disc is forced out, causing the disc to dry out and wear down prematurely. Eventually the joints degenerate into a condition called degenerative joint disease. You may know this as arthritis. (Vertebral subluxation = misalignment, abnormal motion, seized joints)
That's the problem! Constant lifting, bending, poor posture, etc., put consistent stress on your joints. Often, major symptoms can come after a warnings like stiffness, achiness, muscle pulls or spasms, but very commonly there is no warning at all!
Regular chiropractic care can help relieved the small, unfelt subluxations before neglect turns them into major disasters. What are you waiting for? Basically, there are three types of conditions:
If a condition which is new and acute is left uncorrected, it can become chronic. If a chronic condition is left uncorrected, it can become permanent. Pain killing drugs only mask your symptoms. Why not find out for yourself, and join the millions of others who have already learned what modern, gentle, drugless chiropractic can do? Remember: Pain is a symptom that tells you that something is wrong. Chiropractic does more than mask the symptoms: it corrects the underlying cause of the problem to help your body heal itself naturally. Do you know someone who would benefit from this information? Please feel free to forward this message. Have a question? Email me personally at [email protected] Dr. Wayne Coghlan: ChiropractorFrequently Asked Questions
WHERE IS MY OFFICE?
DO YOU NEED A MEDICAL REFERRAL?
WHAT ARE MY FEES?
WHAT HAPPENS AT YOUR FIRST VISIT?
DO I TAKE X-RAYS?
WHAT’S HAPPENS NEXT?
HOW LONG WILL IT TAKE UNTIL YOU ARE BETTER?
WHAT TYPE OF TREATMENT DO I USE?
HOW DOES MANIPULATION WORK?
IS MANIPULATION SAFE?
DOES IT HURT?
DO YOU NEED TO KEEP COMING BACK?
DOES OHIP COVER ANY OF THE COST?
DO WE ACCEPT PRIVATE INSURANCE?
I’M NOT SURE THAT CHIROPRACTIC CAN HELP ME!
CAN I HAVE A NO COST CONSULTATION?
WHAT IS MY PHONE NUMBER? Dr. Wayne Coghlan [email protected] (c) 705 446 7003 |
Dr. Wayne CoghlanI am a graduate of the University of Guelph School of Human Kinetics, and then the Canadian Memorial Chiropractic College, with further education in Sports Sciences, and have completed a Master's degree in Counselling Psychology. Categories
All
|

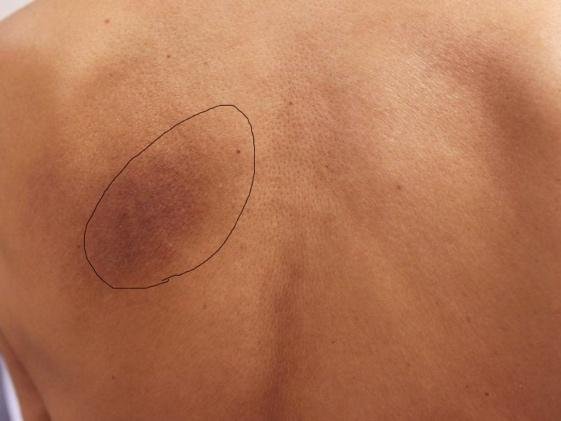
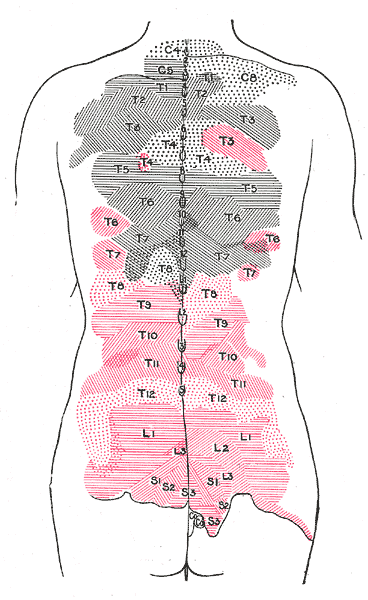
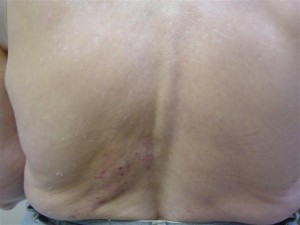



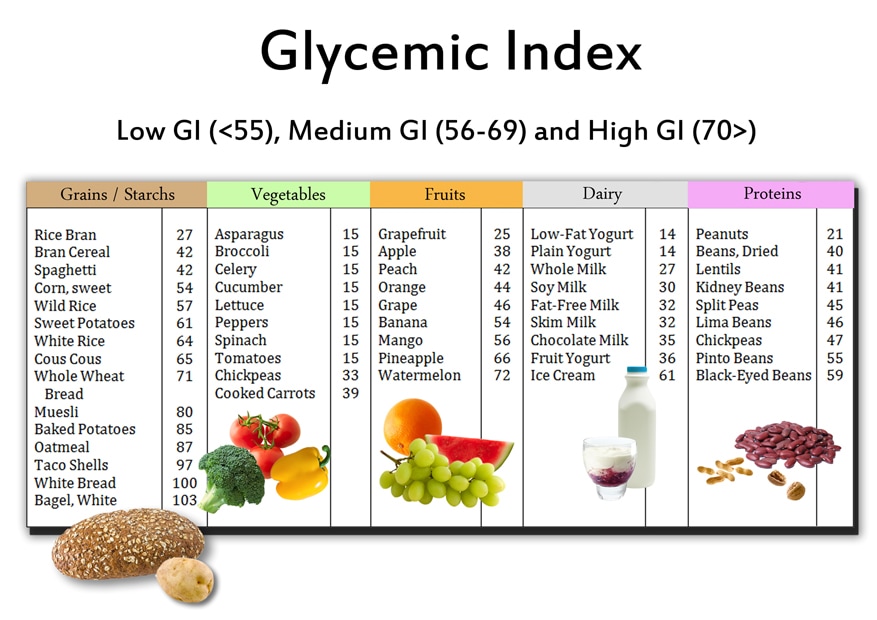
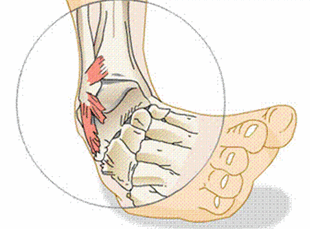












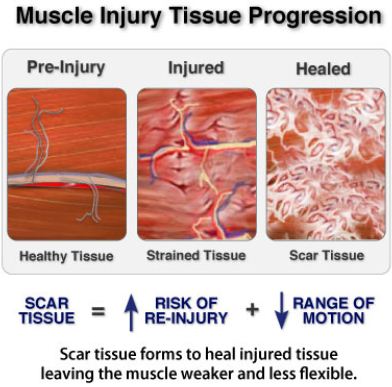

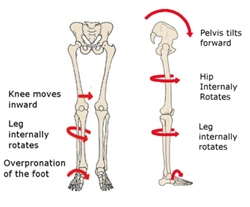

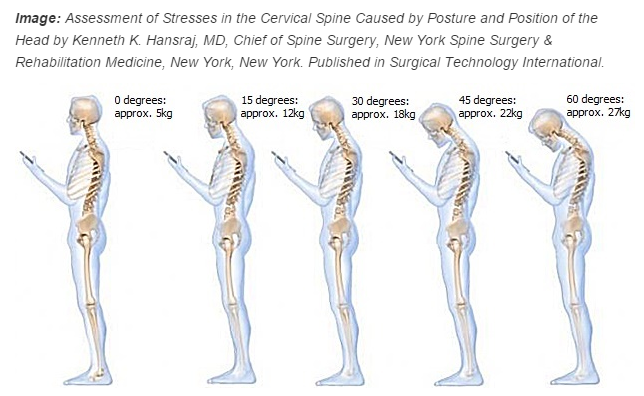
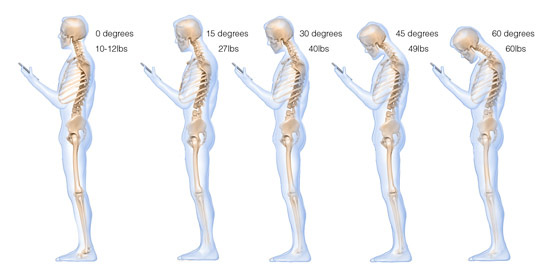

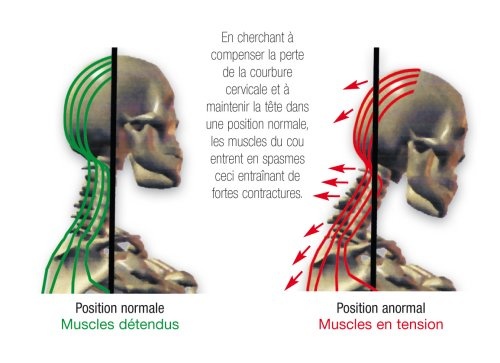





 RSS Feed
RSS Feed


 Dr. Wayne Coghlan: Chiropractor / Counselling Psychology.
Dr. Wayne Coghlan: Chiropractor / Counselling Psychology.